Fever in the Returned Traveler
Authors: Carlos Franco-Paredes, MD, MPH, Jay Keystone, MD MSc (CTM) FRCPC
OVERVIEW
An estimated 15% to 70% of international travelers returning to the US have a travel-related illness (18,19, 33). The likelihood of developing a medical condition during travel relates to an individual’s past medical history, travel destination, duration of travel, level of accommodation, immunization history, adherence to indicated chemoprophylactic regimens, activities during travel, and especially to his or her history of exposure to infectious agents prior to and during travel (15, 29).
While some illnesses that occur in returned travelers may begin during the travel period, others may occur weeks, months or even years after return. In many cases, travelers may be harboring a pathogen in its incubation phase that becomes clinically evident in the immediate post-travel period (29). In terms of clinical severity, most travel-related illnesses are mild, but between 1 to 5 percent of travelers become sick enough to seek medical care either during or after travel (29,33). Thus, a travel history, particularly travel within the previous 6 months, should be part of the routine medical history in every ill patient, especially in those with fever.
Fever is a frequently reported complaint among returned travelers (13, 16, 28, 34). Recently, the Geosentinel surveillance network, a partnership of the International Society of Travel Medicine (www.istm.org) and the Centers for Disease Control and Prevention, reviewed its data on 24,920 travelers (34). This global surveillance system, concerned with illness/injury of international travelers, reported that twenty-eight percent (6,957) of returned travelers seen at Geosentinel clinics from March 1997 through March 2006, presented with fever as their chief reason for seeking medical care (16). Fever was a marker of a potentially serious illness in up to 26% of these travelers and often resulted in hospitalization.
This chapter reviews the approach to the febrile ill-returned traveler from epidemiological, diagnostic and therapeutic perspectives.
APPROACH TO THE PATIENT
Although fever may be an indication of an infectious, inflammatory, or neoplastic disorder, in a febrile ill- returned traveler fever it is most likely to have an infectious etiology. Indeed, in travelers, fever is often caused by a geographically restricted infection such as malaria, dengue, typhoid fever, hepatitis, to name just a few examples (Table 1) (13, 28, 34). Some of these episodes represent life-threatening conditions such as P. falciparum malaria that, if not treated appropriately and early, may be lethal in non-immune populations. Although ‘fever from the tropics’ does not necessarily have a tropical cause, it should be considered to be ‘malaria until proven otherwise’. Fever may also be due to an infectious syndrome not geographically restricted, such as a urinary or upper respiratory tract infection. Although case series from tropical disease centers show malaria as the primary cause of fever, referral bias is almost certainly involved. If primary care physicians were to be surveyed, it is likely that non-geographically restricted infections would be the most frequent cause of febrile illness in returned travelers. It is always worth keeping in mind that very occasionally, patients may present with a febrile illness due to a medical condition that had no association with travel, except that it manifested coincidentally during the travel or post-travel period.
According to the Geosentinel data base, the largest analysis of syndromic causes of fever in travelers, 35% presented with a febrile systemic illness, 15% had a febrile diarrheal disease, and 14% had fever with a respiratory illness. In this report, causes of fever varied by region visited and by time of presentation after travel (34). Malaria was the most common diagnosis, found in 21% of travelers; falciparum malaria was most frequently found in returned travelers from Africa (Table 2) (16, 34). Ill travelers who returned from sub-Saharan Africa, south-central Asia, and Latin America whose reason for travel was visiting friends and relatives were more likely to develop fever compared to other types of travelers. Both malaria and typhoid fever were seen more frequently in this group. The most frequent geographic-specific causes of fever included malaria, dengue fever, rickettsial infections, and typhoid fever. Several previous but smaller studies have shown similar findings (Table 3) (6, 13, 28, 30, 34).
Focused Medical History in Travelers
In addition to the clinical picture, the pre-travel preparation and exposure histories form the basis of the differential diagnosis (20, 29). The immunization history will often rule out particular entities such as hepatitis A, hepatitis B, yellow fever, meningococcal meningitis and Japanese encephalitis in those who have been immunized (5, 7, 20, 26, 17). On the other hand, a history of typhoid immunization does not rule out infection since the vaccine is only 70% effective (5). A history of malaria chemoprophylaxis should include the name of drug, dose, patient adherence to the regimen, and whether the patient is still on the drug on return. It is extremely rare for a traveler to develop falciparum malaria if the antimalarial drug, dose and adherence are appropriate to national guidelines (3, 8).
CDC: Health Information for Travelers by Country
The exposure history is crucial to the formulation of a differential diagnosis (see Table 4) (19, 29). Eliciting a detailed history of the specific locales visited, the timing of travel relative to the onset of symptoms, the exact arrival and departure dates, and specific risk behavior is essential in determining potential exposure to infectious pathogens and likely incubation period. As noted in Table 4 the exposure history should include a history of contact with animals (including bites), new sexual partners, freshwater, insects (especially ticks and tse tse flies), medical equipment (needles, blood transfusions), and ill-persons (9, 22, 25, 32). Also, a history of ingestion of unpasteurized dairy products or uncooked meat as well as an occupational history might be important for the differential diagnosis (29). Knowledge of infectious disease outbreaks (as reported on ProMed – http://www.promedmail.org) in a specific region where the patient has traveled may be very helpful in pinpointing a probable diagnosis. It is important to remember that particular groups of travelers are considered at higher risk of developing illness after returning to their place of residence (29). Adventure travelers and those persons visiting friends and relatives overseas are at greatest risk for becoming ill, in part because of increased exposure to pathogens. Also, those visiting friends and relatives (VFRs) are less likely to seek pre-travel advice, to take antimalarial prophylaxis, and to receive travel-related vaccinations (1, 2, 4, 23).
Differential Diagnosis
In the practice of travel medicine, narrowing the differential diagnosis of fever in the returned traveler is achieved by identifying the likely causative cause by: 1) obtaining a detailed pre-travel and travel history (15, 29); 2) assessing the constellation of signs and symptoms, including incubation periods (15) (Table 1) and 3) taking a history of specific exposures (9, 22, 25) (Table 4). In addition, the abruptness of the fever onset, fever magnitude and pattern, and associated laboratory findings often point to the probable cause of the fever (12, 15, 29).
For diagnostic purposes, fevers may be viewed as acute, subacute, or chronic, and with or without localizing signs (12). The most frequent health problems in ill returned travelers are persistent gastrointestinal illness (11), 10%; skin lesions/rashes (35), 8%; respiratory infections, 5%-13% (depending on season of travel) (24); and fever in up to 3% (34). Although gastrointestinal upset is the most frequent problem, febrile illness is the most serious since the infection may be life threatening to the patient (malaria or meningococcal meningitis) or a pose a serious public health hazard (tuberculosis, measles, or viral hemorrhagic fevers) (3, 8, 15, 16, 29). A report of 30 Geosentinel travel and tropical medical clinics on six continents has shown significant regional differences in terms of morbidity in various syndromic categories in relation to place of exposure among ill returned travelers (16). For example, dermatologic problems were among the most important diagnosis among those travelers returning from the Caribbean or Central or South America, while the diagnosis of acute diarrhea was more common for those travelers returning from South Central Asia (Table 2) (16). Malaria was identified as one of the three most frequent causes of systemic febrile illness among travelers from any region. Besides malaria, travelers returning from Southern Africa were diagnosed with a rickettsial infection; primarily tick-borne spotted fever. Dengue fever on the other hand, was rarely seen in travelers from Africa but common in those returned from Southeast Asia and the Caribbean.
Most travelers infected abroad become ill within 12 weeks after returning to the United States. However, some diseases, such as malaria, may not cause symptoms for as long as 6-12 months after exposure (Table 1) (31). If travelers become ill after they return home, even many months after travel, they should be advised to tell their physician where and when they have traveled.
Fever patterns are sometimes helpful in dissecting febrile-illnesses in travelers (5, 12, 29). Continuous fever pattern may indicate the possibility of typhoid fever or typhus; remittent fever may indicate tuberculosis, African trypanosomiasis; Intermittent fever may be due to malaria or tuberculosis; and relapsing fever may be due to borreliosis, or malaria. The fever pattern associated with falciparum malaria rarely displays periodicity. A classic alternate day or every third day fever is virtually pathognomonic for malaria, the former P. vivax and the latter P. malariae. In particular, fever in a returned traveler from a malarious area should be considered to be malaria until proven otherwise and a medical emergency; the diagnosis of malaria should be evaluated urgently by appropriate laboratory tests and qualified personnel.
Table 5 displays information about which disease exposures are likely in different geographic regions of the world (10).
Diagnostic Workup
The most frequent "tropical" causes of fever in the returned traveler are malaria, dengue fever, invasive bacterial diarrhea, hepatitis A, typhoid fever, and rickettsial infections (Table 3) (3, 6 13, 16, 28, 30, 34). Non-immune individuals are particularly susceptible to develop severe falciparum malaria and to die from it (8, 27). On the other hand, immigrants from developing countries who live in malaria-free nations and return home to visit friends and relatives in their place of birth are at much higher risk of acquiring malaria. Indeed, this particular group of travelers has the highest proportion of imported malaria (1, 2, 4, 23). The majority of VFRs adults do not take malaria chemoprophylaxis and are not aware that, without repeated exposure, their partial immunity to malaria wanes over time. Their risk is particularly high because they have prolonged stays in their country of origin and often spend time in high-risk areas without taking any personal protective measures against malaria (4, 23).
Malaria is the most frequent infectious cause of death in the returned traveler; death may occur within several days of the onset of symptoms (27). Since all prophylactic antimalarials do not prevent the parasite from entering the liver, even individuals who had adhered to appropriate chemoprophylaxis may still acquire the infection (8). Dormant hypnozoites of P. vivax or P. ovale may be released from the liver into the bloodstream many months or even years after infection occurs. However, 98% of all imported falciparum malaria infections, and 74% of vivax infections present within 2 months of return (28, 31). Also, it is important to remember that more than 90% of imported falciparum infections originate in Sub-Saharan Africa (8, 16). The symptoms of malaria are usually non-specific and, unless periodic fever occurs, cannot be differentiated from the usual flu-like viral illness. Fever, chills (with or without rigors), headache, and myalgia are most common; dry cough and abdominal pain not infrequently accompany these symptoms. As noted above, the fever pattern may be helpful, especially for the benign malarias.
Dengue “breakbone” fever also presents with flu-like symptoms, of which the classical features are fever, severe myalgia, headache, retro-orbital pain, and a maculo-papular rash ![]() . However, in one recent study, only 40% of returned travelers with dengue complained of muscle or bone pain (21). The vast majorities of dengue patients become ill within 7 days of exposure and are afebrile within 7 days of the onset of the illness. Dengue is diagnosed by serology and viral isolation. The infection is most frequently acquired from a day-biting mosquito in SE Asia and the Caribbean, but very rarely in Africa (6, 13, 16, 27, 28, 30, 34).
. However, in one recent study, only 40% of returned travelers with dengue complained of muscle or bone pain (21). The vast majorities of dengue patients become ill within 7 days of exposure and are afebrile within 7 days of the onset of the illness. Dengue is diagnosed by serology and viral isolation. The infection is most frequently acquired from a day-biting mosquito in SE Asia and the Caribbean, but very rarely in Africa (6, 13, 16, 27, 28, 30, 34).
The classical presentation of typhoid fever begins with gradual onset of fever that builds to a crescendo over several days to become a persistent fever, often associated with non-specific temperature/pulse dissociation (29). Additional symptoms usually include headache, cough and, unlike non-typhoidal strains of salmonella, constipation. Almost any fever pattern can be seen in those with enteric fever; as noted above, prior immunization does not exclude the diagnosis since the vaccine is only 70% effective (5). The diagnosis is made by blood cultures that are usually positive during the first week of illness and by stool and urine cultures that become positive during and after the second week of illness.
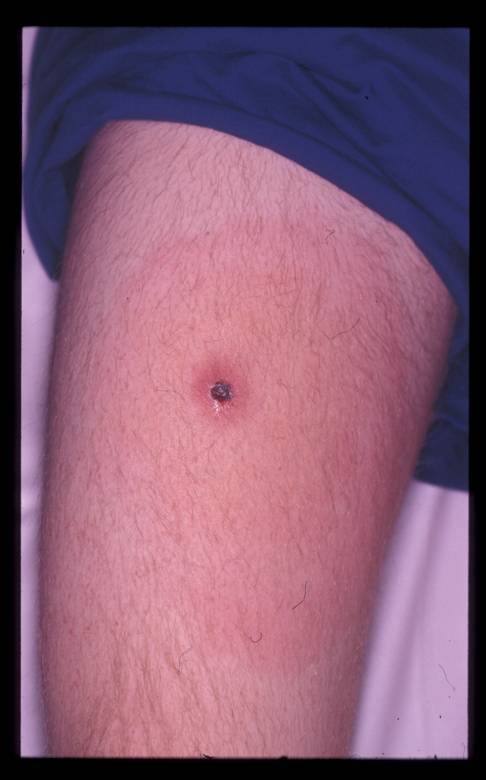
Tick typhus, due to R. africae, is the most frequent cause of fever in a returned traveler from Southern Africa (22). Typical symptoms include fever, localized tender lymphadenopathy, and a macular or papular rash. However, the diagnosis is confirmed clinically by the finding of a tick eschar, a 1-2 cm, black, necrotic lesion with an erythematous margin ![]() . The diagnosis may be missed if the patient’s skin is not fully examined. Diagnosis is by serology, often utilizing acute and convalescent specimens.
. The diagnosis may be missed if the patient’s skin is not fully examined. Diagnosis is by serology, often utilizing acute and convalescent specimens.
A newly returned, ill international traveler should be evaluated by an infectious disease or tropical medicine practitioner. For assistance in finding a provider who practices clinical tropical medicine, one may access the American Society of Tropical Medicine web site for a listing by state at www.astmh.org/scripts/clinindex.asp. In addition, one of the most useful on-line commercial products dealing with international infectious disease issues is the Global Infectious Diseases and Epidemiology Network (GIDEON) (http://www.gideononline.com). This remarkable web-based program utilizes Bayesian principles in clinical decision making to assess illness in returned international travelers (14). The program consists of four modules: one designed to assist in the differential diagnosis of any infectious disease scenario that might occur as a result of a stay any of 220 countries; the second follows the country specific epidemiology of 337 individual diseases; the third, provides a comprehensive review of > 300 anti-infective drugs and vaccines; and the fourth sets out a ranked microbiological identification of bacteria, mycobacterium, and fungi.
Laboratory Diagnosis
Depending upon the exposure history, time course of the illness, and associated signs and symptoms, initial investigations for febrile travelers may include prompt evaluation of peripheral blood smears or a rapid antigen detection method for Plasmodium spp, a complete blood cell count and differential, liver function tests, urinalysis, blood , stool and urine cultures, chest radiography, and specific serologic assays, such as those for the diagnosis of dengue, rickettsial infections, schistosomiasis, leptospirosis, viral hepatitis, HIV etc., (Table 6) (29). For this reason, at the initial assessment it is often valuable to keep a serum sample stored for later testing when acute and convalescent serology are needed. Thick and thin blood films or rapid diagnostic antigen testing for malaria should be repeated twice, 12-24 hours apart if the initial result is negative.
APPROACH TO CASE MANAGEMENT
If the initial malaria blood film or antigen test is negative and the patient is reliable and clinically stable, one might choose to establish close outpatient follow-up and have the malaria test repeated daily. Alternatively, one might consider hospital admission for observation and to obtain serial malaria films. In most cases, a diagnosis of falciparum malaria is an indication for hospital admission. This is not the case for the other 3 malaria species. When reliable malaria blood films or rapid diagnostic testing is not available, treatment for worst case scenario, chloroquine-resistant falciparum malaria, may be a reasonable option in a severely ill patient. In addition, while awaiting test results when the diagnosis is uncertain in a severely ill patient, consideration should be given to starting the patient on broad spectrum antibiotics such as a third generation cephalosporin (i.e. ceftriaxone) or ciprofloxacin plus doxycycline.
CONCLUSION
The investigation of a febrile traveler recently returned from the developing world requires detailed knowledge of the patient’s pre-travel preparation, travel itinerary and exposure history. In addition, knowledge of the global epidemiology of infectious disease and the techniques required to make a diagnosis are invaluable. In many cases, the etiology of the febrile illness will not have a destination-related cause and often the illness will be self-limited without a diagnosis being confirmed. However, the workup-of such patients should always be considered a medical emergency and, where indicated, ”malaria until proven otherwise”. Infectious disease or tropical medicine specialists should be consulted when such expertise is required.
REFERENCES
1. Angell SY, Cetron MS. Health disparities among travelers visiting friends and relatives abroad. Ann Intern Med. 2005; 142:67-72. [PubMed]
2. Angell SY, Behrens RH. Risk assessment and disease prevention in travelers visiting friends and relatives. Infect Dis Clin North Am 2005;19:67-72. [PubMed]
3. Ansart S, Perez L, Vergely O, Danis M, Bricaire F, Caumes E. Illnesses in travelers returning from the tropics: A prospective study of 622 patients. J Trav Med 2005;12: 312-318. [PubMed]
4. Bacaner N, Stauffer B, Boulware DR, Walker PF, Keystone JS. Travel medicine considerations for North American immigrants visiting friends and relatives. JAMA 2004;291:2856-2864. [PubMed]
5. Basnyat B, Maskey AP, Zimmerman MD, Murdoch DR. Enteric (typhoid) fever in travelers. Clin Infect Dis 2005;15 :1467-1472. [PubMed]
6. Bottieau E, Clerinx J, Schrooten W, Van den Enden E, Wouters R, Van Esbroeck M, et al. Etiology and outcome of fever after a stay in the tropics. Arch Intern Med 2006; 166: 1642-1648. [PubMed]
7. Centers for Disease Control and Prevention. Fatal yellow fever in a traveler returning from Amazonas, Brazil, 2002. MMWR. 2002; 51:324-325. [PubMed]
8. Centers for Disease Control and Prevention. Malaria Surveillance – United States, 2005. MMWR 2007; 56 (SS06): 23-38. [PubMed]
9. Centers for Disease Control and Prevention. Update: outbreak of acute febrile illness among athletes participating in Eco-Challenge-Sabah 2000—Borneo, Malaysia, 2000. MMWR. 2001; 50:21-24. [PubMed]
10. Centers for Disease Control and Prevention. Geographic distribution of potential health hazards to travelers. Travelers Health Yellow Book 2007-2008. Ed. Arguin P, Kozarsky P, Reed C. Centers for Disease Control and Prevention, Atlanta GA: 70-73.
11. Connor BA. Sequelae of traveler's diarrhea: focus on postinfectious irritable bowel syndrome. Clin Infect Dis. 2005 1;41 Suppl 8:S577-86. [PubMed]
12. Cunha BA. The clinical significance of fever patterns. Infect Dis Clin North Am 1996;10:33-42. [PubMed]
13. Doherty JF, Grant AD, Bryceson AD. Fever as the presenting complaint of travellers returning from the tropics. QJM. 1995; 88:277-281. [PubMed]
14. Edberg S. Global Infectious diseases and Epidemiology Network (GIDEON): A world wide web-based program for diagnosis and informatics in infectious diseases. Clin Infect Dis 2005;40:123-126. [PubMed]
15. Franco-Paredes C. The Post-travel period. IN: Arguin P, Kozarky P, Reed C. CDC Health Information for International Travel 2008. Centers for Disease Control and Prevention, Elsevier, Mosby 2007.
16. Freedman DO, Weld LH, Kozarsky PE, et al. Spectrum of disease and relation to place of exposure among ill returned travelers. N Engl J Med 2006; 54:119-130. [PubMed]
17. Freedman DO, Leder K. Influenza: changing approaches to prevention and treatment in travelers. J Travel Med 2005;12:36-44. [PubMed]
18. Hill DR. Health problems in a large cohort of Americans traveling to developing countries. J Travel Med. 2000;7(5):259-266. [PubMed]
19. Hill DR. The burden of illnesses in international travelers. N Engl J Med 2007; 352: 115-117. [PubMed]
20. Hill DR, Ericsson CD, Pearson RD, Keystone JS, Freedman DO, Kozarsky PE, et al. The practice of travel medicine: Guidelines by the Infectious Disease Society of America. Clin Infect Dis 2006:43;1499-1539. [PubMed]
21. Jelinek T, Muhlberger N, Harms G, Grobusch MP, Knobloch J, Bronner U, et al. Epidemiology and clinical features of imported dengue fever in Europe: sentinel surveillance data from TropNetEurope. Clin Infect Dis 2002; 35 (9) : 1047-1052. [PubMed]
22. Jensenius M, Fournier PE, Raoult D. Rickettsiosis in International Travelers. Clin Infect Dis 2004; 39: 1493-1499.[PubMed]
23. Leder K, Tong S, Weld L, Kain KC, Wilder-Smith A, von Sonnenburg F, et al. Illness in travelers visiting friends and relatives: a review of the GeoSentinel surveillance network. Clin Infect Dis 2006;43:1185-93. [PubMed]
24. Leder K, Sundararajan V, Weld L, et al, for the GeoSentinel Surveillance Group. Respiratory tract infections in travelers: a review of the GeoSentinel surveillance network. Clin Infect Dis. 2003; 36:399-406. [PubMed]
25. Matteelli A, Carosi G. Sexually transmitted diseases in travelers. Clin Infect Dis. 2001; 32:1063-1067. [PubMed]
26. Mutsch M, Spicher VM, Gut C, Steffen R. Hepatitis A virus infections in travelers, 1988-2004. Clin Infect Dis 2006; 42: 490-497. [PubMed]
27. Newman RD, Parise ME, Barber AM, Steketee RW. Malaria-related deaths among U.S. travelers, 1963-2001. Ann Intern Med 2004; 141: 547-555. [PubMed]
28. O'Brien D, Tobin S, Brown GB, Torresi J. Fever in returned travelers: review of hospital admissions for a 3-year period. Clin Infect Dis. 2001; 33:603-609. [PubMed]
29. Ryan ET, Wilson ME, Kain KC. Illness after international travel. N Engl J Med. 2002; 347:505-16. [PubMed]
30. Roberts MTM, Lever AML. An analysis of imported infections over a 5-year period at a teaching hospital in the United Kingdom. Travel Med Infect Dis 2003; 1: 227-230.
31. Schwartz E, Parise M, Kozarsky P, Cetron M. Delayed onset of malaria-Implications for chemoprophylaxis in Travelers. N Engl J Med 2003; 349:1510-1516. [PubMed]
32. Schwartz E, Kozarsky P, Wilson M, Cetron M. Schistosome infection among river rafters on Omo River, Ethiopia. J Travel Med. 2005;12:3-8. [PubMed]
33. Steffen R, Rickenbach M, Wilhelm U, et al. Health problems after travel to developing countries. J Infect Dis. 1987; 156:84-91. [PubMed]
34. Wilson ME, Weld LH, Boggild A, Keystone JS, Kain KC, van Sonnenburg F, et al. Fever in returned travelers results from the GeoSentinel surveillance network. Clin Infect Dis 2007; 44: 1560-1568. [PubMed]
35. Wilson ME, Chen LH. Dermatologic infectious diseases in international travelers. Curr Infect Dis Rep. 2004; 6:54-62.[PubMed]
Tables
Table 1: Incubation Periods of Frequency Reported Febrile Syndrome in Returned Travelers Compiled from Various Reports (3, 6, 13, 16, 28, 30, 34)
Incubation Period |
Syndromes |
Etiologies |
|---|---|---|
< 2 weeks |
Fever with initial Non-Specific Signs and Symptoms
Fever and Coagulopathy
Fever and Central Nervous System Involvement
Fever and Pulmonary Involvement
Fever and Skin Rash |
Malaria, dengue, scrub typhus, spotted group rickettsiae, acute HIV, acute hepatitis C,Campylobacter, salmonellosis, shigellosis, East African trypanosomiasis, leptospirosis,relapsing fever
Meningococcemia, leptospirosis, and other bacterial pathogens associated with coagulopathy, malaria, viral hemorrhagic fevers
Malaria, typhoid fever, rickettsial typus(epidemic caused by Rickettsia Prowazecki),meningococcal meningitis, rabies, arboviral encephalitis, East African trypanosomiasis, encephalitis or meningitis due to worldwide distributed know pathogens, angiostrongyloidiasis, rabies
Influenza, pneumonia due to typical pathogens, Legionella pneumoniae, acute histoplasmosis, acute coccidioidomycosis, Q fever, SARS
Viral exanthems (rubella, varicella, mumps,human herpesvirus-6), dengue, spotted or typhus group rickettsiosis, typhoid fever, parvovirus B19 |
2 to 6 Weeks |
Various Syndromes (Fever with Pulmonary, Dermatologic, Central Nervous System, or other sites Involvement) |
Malaria, tuberculosis, hepatitis A, hepatitis B,hepatitis E, visceral leishmaniasis, acute schistosomiasis, amebic liver abscess, leptospirosis, African trypanosomiasis, viral hemorrhagic fevers, Q fever, acute American trypanosomiasis |
> 6 Weeks |
Various Syndromes (Fever with Pulmonary, Dermatologic, Central Nervous System, or other sites Involvement) |
Malaria, tuberculosis, hepatitis B, hepatitis E, visceral leishmaniasis, filariasis,onchocerciasis, schistosomiasis, amebic liver abscess, chronic mycoses, African trypanosomiasis, rabies, typhoid fever |
* Adapted from References 15, 29.
Table 2. Fever in Returned Travelers Geosentinel Global Surveillance Network *
Etiology |
Caribbean
|
Central America |
South America |
Sub-Saharan Africa |
South Asia |
Southeast Asia |
|---|---|---|---|---|---|---|
<1 |
13 |
13 |
62 |
14 |
13 |
|
23 |
12 |
14 |
<1 |
14 |
32 |
|
Mononucleosis |
7 |
7 |
8 |
1 |
2 |
3 |
0 |
0 |
0 |
6 |
1 |
2 |
|
2 |
3 |
2 |
<1 |
14 |
3 |
* Geosentinel sites are specialized travel or tropical-medicine clinics on six continents that collect clinician-based surveillance data on travel related diseases
Table 3. Causes of Fever in Returned Travelers Reported in Various Clinical Series
Etiology ^ |
Roberts30 (N=147) |
Doherty13 (N=195) |
O’Brien28 (N=232) |
Wilson34* (N=6957) |
Bottieau6 (N=1842) |
|---|---|---|---|---|---|
| Malaria ** | 48% | 42% | 27% | 21% | 33.5% |
| Dengue fever | 5% | 6% | 8% | 6% | 3% |
| Typhoid fever | 6% | 2% | 3% | 2% | 0.8% |
| Respiratory infection*** | 4 | 15% | 23% | 24% | 10.5% |
| Urinary tract infection | 2 | 3% | 1% | 1% | 3.4% |
| Viral hepatitis | 13% | 3% | 3% | 1% | 0.6% |
| Rickettsial disease | 1% | 1% | 2% | 2% | 4% |
| Tuberculosis | 1 | 1% | 0.4% | - | 1.6% |
| Gastroenteritis | 7% | 7% | 14% | 2% | 6.2% |
| Leptospirosis | 1% | - | - | - | 0.3% |
| Viral Syndrome | 18% | - | - | 3% | - |
| Unspecified febrile illness | - | 25% | 9% | 22% | 24% |
** All Plasmodium spp.
^ Columns do not add up to 100% since patients may have more than 1 diagnosis*** Including upper and lower respiratory infections
Table 4. Exposure History and the Conditions to be Considered
Activity |
Disease risk
|
|---|---|
Food
|
Hepatitis, bacterial enteritis, trichinosissalmonellosis Listeriosis, brucellosis, bovine TB |
Fresh water |
|
Sexual contact, tattoing, piercing |
|
Arthropod bites
|
Typhus, borreliosis (relapsing fever) |
Animals |
Rabies, Q-fever, plague, tularemia, borreliosis, histoplasmosis (caves), anthrax |
Ill persons |
Viral hepatitis, typhoid, influenza, viral hemorrhagic fever |

Table 5. Disease Distribution of Relevant Causes of Fever in the Returned Traveler According to Region of the World*
| REGION | Dengue | Viral Hemorrhagic Fevers | Hepatitis A | HIV | Typhoid | Leptospirosis | Malaria | Rickettsiae |
|---|---|---|---|---|---|---|---|---|
| NA | L | W | S | S,H | S | S | W | |
| CEWA | S,H | S,H | W | W,H | S,H | W.H | W,H | W |
| SA | S | S,H | W,H | S | S | S,H | W,H | |
| NAM | L | S,H | S | L | W,H | S | ||
| MCA | S,H | W | S | S,H | W,H | S | S | |
| CA | S,H | S,H | S | S | W,H | S | S | |
| TSA | S,H | S,H | W | S | S,H | W,H | S,H | S |
| TESA | L | S,H | S,H | S | S | S | S | L |
| EA | S,H | W,H | S | S | W | S | W | |
| SEA | W,H | W,H | S,H | W | W,H | W | W,H | |
| SOA | S,H | W | S,H | W,H | W,H | W,H | W,H | |
| ME | S,H | L | W | S | S | S | S | S |
| WE | S,H | S | L | S | S | |||
| EUNA | W,H | S,H | S,H | S | S | S | ||
| ASP | S,H | S,H | S | S | S | S,H | S |
NA: North Africa; CEWA: Central, East, West Africa; SA: Southern Africa; NAM: North America; MCA: Mexico, Central America; CA: Caribbean; TSA: Tropical South America; TESA: Temperate South America; EA: East Asia; SEA: Southeast Asia; SOA: South Asia; ME: Middle East; WE: Western Europe; EUNA: Eastern Europe and Northern Asia; ASP: Australia and South Pacific.
*Adapted from Reference 33. For further information on risk of health hazards by region see Chapter 3, Health Information for Travelers CDC, Yellow Book.
Table 6. Laboratory and Imaging Studies to Consider in a Returned Traveler with Fever
| Primary Laboratory Testing | Primary Radiographic Testing |
|---|---|
|
|
| Secondary Laboratory Testing | Secondary Radiographic Testing |
|
|
Figure 1. Classic Dengue Rash in a Returned Traveler with Fever
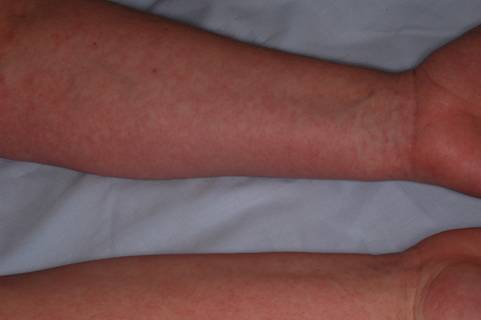
Figure 2. Eschar Associated to Rickettsia africae Tick Bite Fever
Guided Medline Search For:
Reviews
Hill DR, et al. The Practice of Travel Medicine: Guidelines by the Infectious Disease Society of America. Clin Infect Dis 2006;43:1499-1539.
