
Lymphadenopathy - Causes
(Localized/General and Infectious/Non-infectious)
DIFFERENTIAL DIAGNOSIS
Local Adenopathy
Localized lymphadenopathy can suggest the site of infection, although not
necessarily the original source of infection. For example, the sexually
transmitted disorders usually affect the genitalia and inguinal lymph nodes, but
if the primary lesion (e.g., a syphilitic chancre) is located elsewhere, e.g.,
the mouth, the adenopathy will be in the cervical area. Similarly, diseases
spread by insect vectors will cause adenopathy in the area corresponding to the
site of inoculation (Table 3).
Table 3: Localized and Generalized
Lymphadenopathy
|
LOCALIZED LYMPHADENOPATHY |
|
Cervical adenopathy |
Pharyngitis
- Virus (adeno,
enteto, parainfluenza, HIV, herpes simplex, others)
- Group A Streptococcus
- Arcanobacterium
hemolyticum
- Mycoplasma
|
|
Infectious mononucleosis (EBV, CMV)
|
|
Diphtheria (Corynebacterium
diphteriae) |
|
Toxoplasmosis |
|
Fusobacterium
Infection |
|
Mycobacterial adenitis (M.tuberculosis, M.avium
complex etc) |
|
Kikuchi's disease |
|
Kawasaki's disease |
|
Occipital adenopathy |
Nonspecific scalp infection |
|
Rubella |
|
Peripheral adenopathy |
Location varies with inoculation site.
- Bacterial adenitis
- Bartonella henselae (Cat-scratch
disease)
- Tularemia (Franciscella Tularensis)
- Plague (Yersinia pestis)
- Rat-bite
fever (Streptobacillus
moniliformis, Spirillum minus)
- Rickettsioses (Orientia
Tsutsugamushi, Rickettsia akari, Spotted fever group Rickettsial
Infections)
|
Usually axillary or epitrochlear
- Sporotrichosis
- Herpes zoster infection
- Herpetic whitlow (HSV1, 2)
|
|
Inguinal |
Primary syphilis
|
|
LGV (lymphogranuloma venereum) Chlamydia
trachomatis |
|
Chancroid Haemophilus ducreyi |
|
Granuloma inguinale Klebsiella granulomatis
|
|
Genital herpes infection, Herpes simplex
type 2 |
| |
|
GENERAL LYMPHADENOPATHY |
- Infectious mononucleosis
- EBV
- Rubella
- CMV
- HIV
- Hepatitis virus
- Measles
- Dengue
- Toxoplasmosis
- Tularemia (Franciscella
tularensis)
- Brucella
- Histoplasmosis
- Secondary syphilis
- Miliary tuberculosis
|
Cervical Adenitis
Cervical adenitis is usually secondary to pharyngitis by respiratory viruses
or by group A streptococcus. Group A streptococcal infection (Streptococcus pyogenes) of the pharynx can cause tender anterior cervical adenopathy. The
appearance of the pharynx, the presence of exudative material, and the character
of the nodes are all nonspecific.
Epstein Barr Virus:
Infectious mononucleosis is usually associated with a pharyngitis that may be exudative. Cervical adenitis involving both the anterior
and posterior cervical nodes is almost always present. Mononucleosis should be
considered as a cause of pharyngitis in the adolescent or young adult. The
lymphadenopathy may not be localized to just the cervical region but may be
generalized. Splenomegaly, palatal petechiae, supraorbital edema and a
generalized maculopapular rash may occur. Hepatomegaly and/or abnormalities of
liver function are common in infectious mononucleosis.
Cytomegalovirus:
Cytomegalovirus (CMV) infection can mimic infectious
mononucleosis, but the Monospot and EBV antibody tests are negative. The
pharyngitis and cervical adenopathy in CMV infection is less pronounced than in
EBV mononucleosis.
Rarer bacterial etiologies of pharyngitis include Neisseria gonorrhoae
(severe pain but minimal erythema), A. hemolyticum (may be accompanied by a
diffuse erythema) and Yersinia species (sometimes suggested by gastrointestinal
symptomatology).
Mycobacterial Species:
Scrofula (tuberculous cervical lymphadenitis) presents
as painless, enlarged and matted lymphnodes; fluctuation may develop in some
nodes. Spontaneous drainage of caseous material onto the skin surface (scrofuloderma)
may occur. The node enlargement is usually unilateral and isolated to one group
of nodes. The disease is usually located to the lymph nodes only. This syndrome
is typically seen in children who are otherwise healthy and have a negative
chest x-ray. The responsible pathogens are M. scrofulaceum and M. avium
complex
(MAC). Mycobacterial cervical adenitis in young adults, aged 20 to 40, is
usually caused by classical M. tuberculosis
 .
.
|
Vietnamese man with tuberculosis lymphadenitis |
|
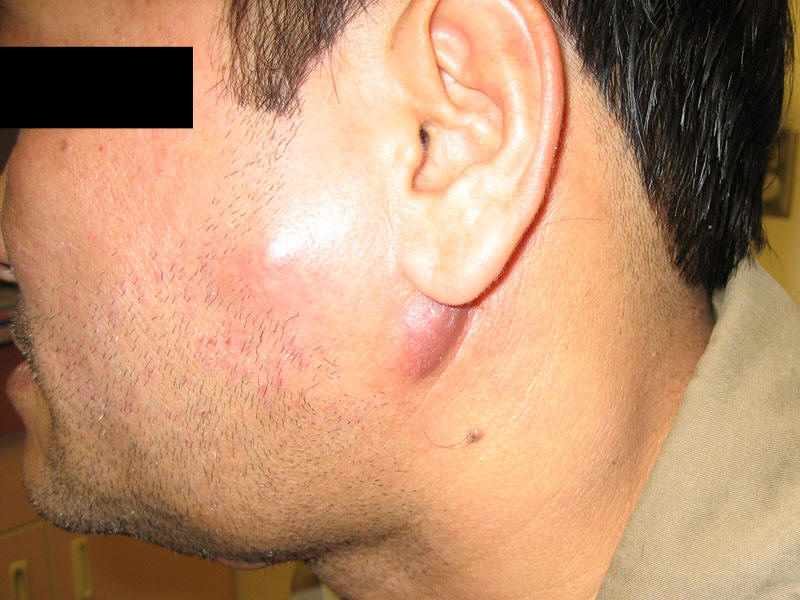 |
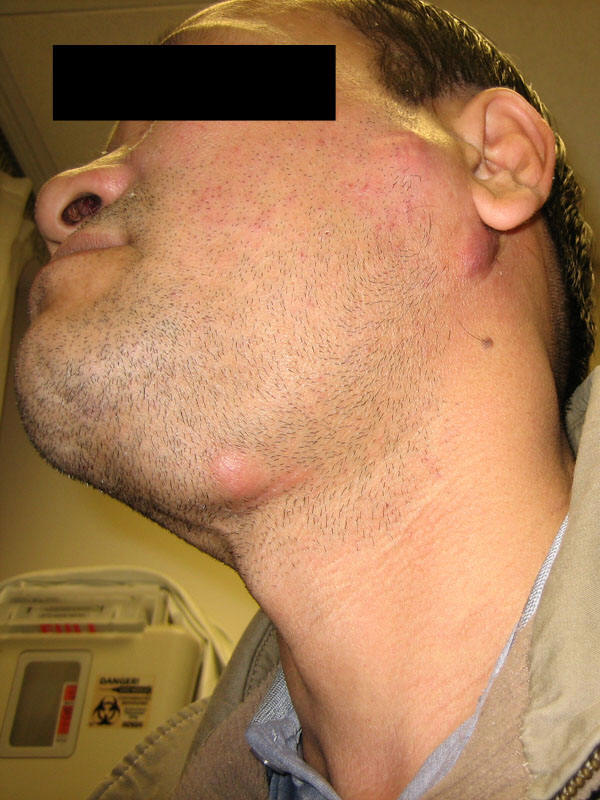 |
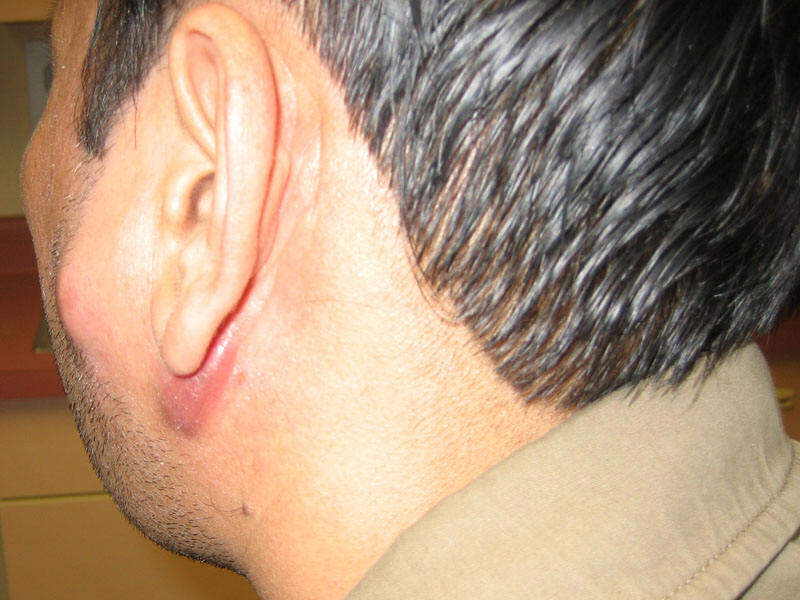 |
Active tuberculosis is usually present elsewhere in the body, although the
chest x-ray may show no evidence of tuberculosis in 50 percent of patients. Lymph
nodes in mycobacterial infections may be large and matted together and are
usually painless. The course of tuberculosis adenitis is generally chronic.
Although the caseating granulomas are the classical findings, this is not
diagnostic unless the organisms can be identified. Specimens for cultures must
be taken at the time of excision or biopsy. A positive tuberculin skin test can
suggest the diagnosis. Tuberculosis adenopathy caused by M. tuberculosis usually
responds to antituberculosis therapy alone, but excision is generally required
to treat disease caused by atypical mycobacteria.
Corynebacterium
Diptheriae:
Diphtheria is an extremely rare cause of acute
cervical lymphadenopathy except in developing countries. History of immunization
is crucial. Diphtheria should be suspected in any nonimmunized patient with a
pharyngitis accompanied by a gray pseudomembrane that is difficult to remove.
Cervical adenopathy and edema of the anterior neck and submandibular areas
frequently occur with this form of pharyngitis. Other much more frequent causes
of a pharyngeal pseudomembrane are EBV, Streptococcus group A, fusobacterium,
Candida albicans, and upper respiratory tract viral pathogens.
Kawasaki’s Disease:
The mucocutaneous lymph node syndrome (MLNS) is
characterized by protracted fever (longer than five days) associated with
cervical adenopathy, conjunctival injection, redness of pharynx and lips, and
diffuse scarlatiniform rash including the palms and soles, with subsequent
desquamation. The disease may be mistaken for Group A streptococcal scarlet
fever, but the diagnostic studies for streptococcal infection are negative and
penicillin is ineffective. The fatality rate (about 1%) is related to coronary
arteritis.
Kikuchi’s Disease:
Kikuchi’s disease (also called Kikuchi-Fujimoto disease or
Kikuchi’s histiocytic necrotizing lymphadenitis) occurs predominately in
females. Clinical features are characterized by fever, cervical lymphadenopathy,
and transient skin rash. Signs and symptoms usually resolve spontaneously within
one to four months. The definitive diagnosis of Kikuchi’s disease is made by
lymph node biopsy. Histological findings show follicular hyperplasia in early
phase, the presence of blast cells in the “proliferative phase”, and necrosis
with histiocytes in the “necrotizing phase”. This syndrome is
more common in Asia than elsewhere.
Other Nonbacterial
Causes:
Adenovirus and herpes simplex type 1 can produce
severe exudative and ulcerative pharyngitis, as can primary HIV infection.
Mycoplasma may cause a mild pharyngitis similar to viral infection. Cervical
adenopathy may be mimicked by other inflammatory processes of the neck including
parotitis and Ludwig’s angina.
Occipital Lymphadenopathy
Local infections of the scalp such as pediculosis capitis, impetigo, and
ringworm may cause lymphadenopathy in the occipital region. Systemic infections
such as syphilis and tuberculosis may enlarge occipital nodes, but usually
involve other nodes more dramatically. Rubella virus causes generalized
infection that involves occipital nodes; this adenopathy may precede the rubella
rash by several days. The nodes, although generalized, usually predominate in
occipital, mastoid, and posterior cervical locations. Rubeola also can cause
this pattern of adenopathy in addition to rash, fever, and upper respiratory
symptoms.
Peripheral Axillary and Epitrochlear Adenopathy
Enlargement of the
axillary and epitrochlear or inguinal nodes occurs most frequently from
bacterial infection on the extremities. Repeated trauma to the lower extremities
can lead to inguinal lymphadenopathy. Nonspecific inguinal adenopathy is common
such that biopsy of the inguinal nodes is usually nondiagnostic. If other nodes
are enlarged and accessible, biopsy may be more productive there.
Group A Streptococcus:
Group A streptococcal infection of the extremities may
produce cellulitis and lymphangitis with regional adenopathy. Fever and
superficial red streaks may occur, with painful and tender swollen regional
nodes.
Francisella
Tularensis:
Tularemia of the ulceroglandular type is most
frequently associated with the bite of a tick or deerfly, or with contact with
the carcass of an infected animal. The site of inoculation is characterized by
an ulcerating papule. Regional adenopathy, the location of which depends on the
inoculation site, is manifested by hot, large, fluctuant, and tender lymph nodes
that may suppurate and drain spontaneously. On the other hand, the node
enlargement may at times be much less dramatic and recognized only after very
careful physical examination.
Bartonella
Species:
Cat Scratch Disease may be manifest by localized adenitis
in the epitrochlear, axillary, and inguinal areas depending on the site of the
scratch or bite. The etiology of cat-scratch disease is Bartonella henselae, a
fastidious gram-negative rod. Facial lesions may be associated with cervical or
auricular adenopathy. The primary lesion is a tender papule that is frequently
capped by a vesicle. Regional nodes then become enlarged and tender, and the
overlying skin may be red. If the node becomes fluctuant, it should be aspirated
but not incised. Aspiration may reduce local pain with a dramatic lysis of
fever.
Yersinia
Pestis:
The most common form of disease, bubonic plague, is
manifested by high fever and systemic toxicity, as well as by an erythematous,
edematous matted group of inguinal or axillary nodes that can suppurate and
drain spontaneously. The inoculating flea bite is usually not apparent. The
enlarged lymph node, the bubo, is extremely tender. The diagnosis can be made by
culture of an aspirated lymph node.
Spirillium
Minus:
Rat-bite fever caused by S. minus may cause rash, lead to
the syndrome of a swelling at the site of the bite, regional adenopathy, and
fever. The local infected nodes are tender, firm, and freely movable. One to
four weeks after the bite, the local lesion flares again as the systemic phase
of the illness begins. Fever, generalized rash, and arthritis occur. This
infection is more common in Asia and is called Sodoku in Japan. In the other
form of rat-bite fever, which is more common in the Western hemisphere is caused
by Streptobacillus moniliformis, adenopathy is not prominent.
Sporotrichum
Schenkii:
Sporotrichosis is often manifest by primary lesion of
the upper extremities and the characteristic intermittent hard red lumps along
the lymphatics. The nodes then enlarge and the cutaneous nodules may ulcerate.
Pain and fever are absent, and the streaking seen in acute bacterial
lymphangitis is rare. Sporotrichosis is diagnosed by culture of the nodules,
since neither serology nor scrapings or the lesions for staining are helpful.
Usually the infection stays localized but requires a long time for resolution.
Although rare, primary cutaneous coccidioidomycosis, nocardiosis, and
blastomycosis may mimic local sporotrichosis.
Herpes Zoster:
Most commonly seen on the trunk, herpes zoster causes a
syndrome of clustered vesicles in a unilateral segmental distribution,
frequently preceded and accompanied by marked paresthesias, mild fever, and
headache. Signs and symptoms usually precede the rash by a few days but at times
by as long as one to two weeks. Regional adenitis is a consistent feature of
herpes zoster. The nodes are nontender and freely movable.
Herpes Simplex (Herpetic whitlow):
Epitrochlear and axillary adenopathy may
be a complication of herpetic whitlow, an infection of the pulp of a finger
caused by Herpes simplex, usually type 1. This primary lesion is usually very
painful.
Rickettsioses:
Rickettsial infection present with fever, headache, myalgic
and regional lymphadenopathy. The etiologies include Oritentia tsutsugamushi
(Scrub Typhus), Rickettsia akari (Rickettsialpox), and other spotted fever group
Rickettsial infections including R. australis (Queensland tick typhus), R. honei
(Flinders Island spotted fever), R. conorii (African tick bite fever), R.
sibirica (Siberian tick typhus), R. sibirica mongolotimonae
(Lymphangitis-associated rickettsiosis), R. slovaca (Tick-borne
lymphadenopathy).
Inguinal Adenopathy
Many sexually transmitted infections
are responsible for inguinal lymph node enlargement. Frequently, a genital ulcer
accompanies the adenopathy, producing the “ulcer-adenopathy” syndrome.
Treponema
Pallidum:
Syphilis often presents as a painless skin lesion, the
chancre, usually on the external genitalia, with enlarged freely movable, firm,
nonsuppurating, and painless inguinal nodes. The chancre heals in two to six
weeks, but the lymphadenopathy may persist for months. Diagnosis of primary
syphilis is made by a characteristic lesion and serology.
Haemophilus
Ducreyi:
Unlike syphilis, the genital ulcers and inguinal nodes
of chancroid are tender and painful. If untreated, the nodes may suppurate and
rupture to form a large single ulcer. This last complication may be prevented by
aspiration when the node is tense.
Lymphogranuloma
Venereum (LGV):
Chylamydia trachomatis is the cause of
Lymphogranuloma vereum, a genital ulcer disease. Inguinal adenopathy is
prominent in LGV and may progress to multiocular suppuration with multiple
fistulae. At times the inguinal ligament forms a line of cleavage through the
matted nodes, which are enlarged both above and below the ligament (the “Groove”
sign). The primary genital lesion is a single small ulceration that generally
goes unnoticed. It has usually disappeared by the time the lymph node
enlargement occurs. LGV may be accompanied by generalized constitutional
symptoms and is occasionally associated with severe arthralgias, diarrhea, and
hyperglobulinemia. It is rare in developing countries but can be endemic in
tropical countries. PCR of specimens taken from the ulcer is now the most
sensitive diagnostic method.
Klebsiella
Granulomatosis:
Klebsiella granulomatous is the cause of granuloma
inguinale (Donovanosis). The disease is manifested by a painless genital papule
anad nodule that erodes to leave a beefy red granular base. The infection
spreads to the inguinal area and produces a marked subcutaneous swelling. The
lesion is called a “pseudobubo” since it is not really due to lymph node
involvement, but rather to soft tissue granulation and frequently ulceration.
This infection is rare in developing countries.
Herpes Viruses:
Genital herpetic lesions are characteristically multiple,
small erosions on an erythematous base, typically arranged in a cluster. They
are extremely painful and are often accompanied by bilateral or unilateral
inguinal adenopathy.
Generalized Adenopathy
Fever and generalized adenopathy are usually due to viruses, especially EBV
and rubella, and HIV. EBV mononucleosis may also be mimicked by infection with
CMV, Toxoplasmosis gondii and HIV. Acquired or reactivated CMV infection is most
frequent in normal young people, in patients who have had surgery with bypass
(postperfusion syndrome), recipients of blood transfusions, leukocyte infusions
and transplants, and in immunocompromised individuals. Patients with this CMV
syndrome may present with protracted fever and with moderate hepatic
inflammation along with lymphocytosis and atypical lymphocytes, which occur late
in the course of the disease. Splenomegaly and adenopathy are not always
present. The hepatitis viruses and HHV-6, the cause of roseola infantium, can
also produce lymphadenopathy and a mononucleosis-like illness. Other viruses,
particularly rubella, adenovirus, and dengue can also cause significant
generalized lymph node enlargement (Table 3).
Primary HIV infection causes a mononucleosis-like illness often accompanied
by a diffuse salmon-colored rash that includes the palms and soles.
Lymphadenopathy occurs in 50 to 75 % of patients who develop an acute illness
approximately 3 to 6 weeks after initial exposure to HIV. In the latency period,
persistent generalized lymphadenopathy (PGL) affects between 50 to 70 percent of
HIV patients. The lymph nodes are non tender and affect the nodes in the
cervical, mandible, inquinal and axillary areas.
Lynphadenopathy is found in 5% of acute viral hepatitis. HBV infection in
childhood can be associated with papular dermatitis with enlarged lymph nodes in
the axillary and inguinal regions-the Gianotti-Crosti syndrome. This syndrome
can also occur after infection by EBV, HAV, HCV, CMV, enterovirus, parvovirus,
parainfluenzavirus, rotavirus, respiratory syncytial virus, HIV, HHV-6,
Mycoplasma pneumoniae, beta-hemolytic streptococci, Bartonella henselae,
Borrelia burgdorferi, and following vaccination with influenza virus vaccine,
measles-mumps-rubella vaccine, hepatitis B vaccine, oral polio vaccine or
Japanese encephalitis vaccine.
Toxoplasma gondii:
The most common syndrome seen in acquired symptomatic
toxoplasmosis resembles EBV mononucleosis, with enlarged nonsuppurative lymph
nodes, fever, and maculopapular rash. The nodes in toxoplasmosis are firm,
discreet, freely movable, and at times, painful and tender. The disease has
occasionally been misdiagnosed as Hodgkin’s disease. Frequently the cervical
nodes are the largest, increasing the clinical similarity of this entity to
mononucleosis. Toxoplasmosis can involve the CNS, liver, heart, lungs, or eyes
as target organs. This infection must be considered in patients with an
underlying immunosuppressive disease.
Brucella Species:
Brucellosis is characterized by fever, chills,
hepatosplenomegaly, arthralgia, and leukopenia with relative lymphocytosis.
Sarcoiliitis and spondylitis are common. Small, nontender, cervical and axillary
node enlargements are common. These nodes may show granulomas or a striking
reticuloendothelial hyperplasia with some multinucleate giant cells. Testicular
swelling and/or pain may occur.
Histoplasmosis and fungi:
Disseminated histoplasmosis and other deep fungal
infections are capable of producing widespread lymphadenopathy as part of the
generalized reticuloendothelial reaction to these agents.
Treponema pallidum:
Secondary syphilis is recognized by nontender,
generalized lymphadenopathy with fever and a diffuse nonpruritic maculopapular
rash, which often includes the palms and soles. The nodes may remain palpable
even months after the disappearance of other stigmata of secondary syphilis,
i.e., fever, rash, condylomata, and mucous patches. Pre and postauricular,
occipital and epitrochlear nodes are all frequently enlarged in secondary
syphilis.
Mycobacterium tuberculosis:
Miliary tuberculosis may cause generalized
adenopathy. The typical military pattern on chest x-ray may often be delayed.
Non-Infectious Causes
Many noninfectious disorders include adenopathy among their manifestations,
e.g., lymphoreticular malignancies, collagen vascular diseases, and sarcoidosis
(Table 2). Peripheral non-tender, lymphadenopathy is common in sarcoidosis; the
cervical, axillary, epitrochlear, and inguinal nodes are the most commonly
involved regions. The nodes are non-ulcerative unlike infectious causes.
Table 2: Infections Causing Lymphadenopathy
| Infections |
| Viral |
- Infectious
mononucleosis (Epstein-Barr virus)
-
Cytomegalovirus
- Infectious hepatitis
- Adenovirus
- Herpes simplex, Herpes zoster
- HHV-6 (Human herpesvirus-6)
- HIV
- Human T-lymphotropic
virus
- Rubella
- Measles
|
| Bacterial
|
- Cutaneous infections (Staphylococcus, Streptococcus)
- Cat-scratch fever
- Chancroid
-
Melioidosis
- Tuberculosis
- Atypical Mycobacteria
- Primary and secondary syphilis
|
|
Chlamydial |
|
|
Protozoan |
|
|
Mycotic |
- Histoplasmosis
- Coccidiodomycosis
|
|
Rickettial |
|
|
Helminthic |
|
| Noninfectious Causes |
| Autoimmune |
- Rheumatoid arthritis
- Juvenile rheumatoid arthritis
- Systemic lupus erythematosus
- Dermatomyositis
- Mixed connective tissue disease
- Sjogren’s syndrome
|
| Iatrogenic hypersensitivity |
- Serum sickness
- Drug hypersensitivity
|
| Neoplasm |
|
| Miscellaneous |
- Sarcoidosis
- Amyloidosis
- Vaccine-induced
- Kikuchi's disease
- Hyperthyroidism
- Storage diseases (Gaucher,
Niemann-Pick, Fabry, and Tangier)
- Severe hypertriglyceridemia
-
Kimura’s disease
- Kawasaki disease
- Silicone injection
- Graft vs host disease
- Autoimmune hemolytic anemia
- Gianotti-Crosti syndrome
|
![]() .
. 


