

Cellulitis - Treatment I (Generalized and Individualized Approaches)
Generalized Approach
The existing treatment paradigm is that empiric therapy should provide coverage for the most commonly involved gram-positive cocci. The presence or absence of an abscess as well as recent antibiotic exposures also impacts empiric treatment in light of issues regarding CA-MRSA. Treatment options and common pathogens are detailed in Table 1 for different cellulitis syndromes. Algorithms 1-4 provide extensive detail on dealing with the various types of cellulitis and associated conditions. Whether initial empiric therapy administered parenterally or orally is based on the clinician’s decision and not on evidence-based data which are not available. A list of indications for inpatient antibiotic treatment are listed in Table 4 and includes: comorbidities, signs of systemic toxicity (tachycardia, hypotension), those who cannot tolerate oral antibiotics or those who are not reliable for early follow up should be hospitalized and treated with parenteral therapy. Once symptomatic improvement occurs, therapy can be switched to oral (usually within 2-5 days) to complete 10-14 days course.
Individualized Approach
Although the antibiotic regimens listed in Algorithms 1-4 should be efficacious in most cases of cellulitis in the immunocompetent patient; pivotal epidemiologic and host factors must be reviewed case-by-case so that therapy for less frequent or more resistant pathogens is provided when unique factors are present. In each case, however, empiric coverage should be selected that will provide coverage for beta-hemolytic streptococci and methicillin-sensitive Staphylococcus aureus. The following sections address treatment options in those cases where epidemiologic or host-related factors impact choice of empiric therapy of cellulitis. Treatment options are detailed in Table 1.
Recurrent Abscesses
The major method of controlling
recurrent abscesses
![]() is the use of antibacterial agents to eradicate staphylococcal carriage. There
is scant data available on the efficacy of the various decolonization regimens.
Mupirocin (bactroban) is the most commonly utilized topical antibiotic, often
applied to the nares on the first 5 days of each month for 6 consecutive months.
Chlorhexedine body wash is often used in conjunction with mupirocin, but
tolerating it is challenging due to drying and irritation of the skin.
Decolonization of household contacts may decrease recurrent episodes and should
be considered. If these regimens fail, then low dose systemic antibiotics may be
employed. Daily single dose clindamycin (150 mg) for 3 months has been shown to
be 80% effective in decreasing staphylococcal colonization. Single dose TMP-SMX
or doxycycline for 3 months has also been used, though clinical data is scarce.
Some endorse the previous mentioned systemic antibiotics combined with rifampin
for a shorter course of therapy to attempt to eradicate colonization. Several
small studies have shown that tea tree oil (4% nasal ointment and 5% body wash)
is at least as effective as a mupirocin based regimen. Polysporin may also have
a role in the decolonization process.
is the use of antibacterial agents to eradicate staphylococcal carriage. There
is scant data available on the efficacy of the various decolonization regimens.
Mupirocin (bactroban) is the most commonly utilized topical antibiotic, often
applied to the nares on the first 5 days of each month for 6 consecutive months.
Chlorhexedine body wash is often used in conjunction with mupirocin, but
tolerating it is challenging due to drying and irritation of the skin.
Decolonization of household contacts may decrease recurrent episodes and should
be considered. If these regimens fail, then low dose systemic antibiotics may be
employed. Daily single dose clindamycin (150 mg) for 3 months has been shown to
be 80% effective in decreasing staphylococcal colonization. Single dose TMP-SMX
or doxycycline for 3 months has also been used, though clinical data is scarce.
Some endorse the previous mentioned systemic antibiotics combined with rifampin
for a shorter course of therapy to attempt to eradicate colonization. Several
small studies have shown that tea tree oil (4% nasal ointment and 5% body wash)
is at least as effective as a mupirocin based regimen. Polysporin may also have
a role in the decolonization process.
50 year old male with MRSA abscess of his thigh
Algorithm 1: Empiric Intravenous Antibacterial
Agent Therapy Based on Anatomic Site.

Algorithm 2: Empiric Intravenous Antibacterial Therapy for Community-Acquired Cellulitis Based on Host Status and in Patients without Preceding Antibiotic Therapy.
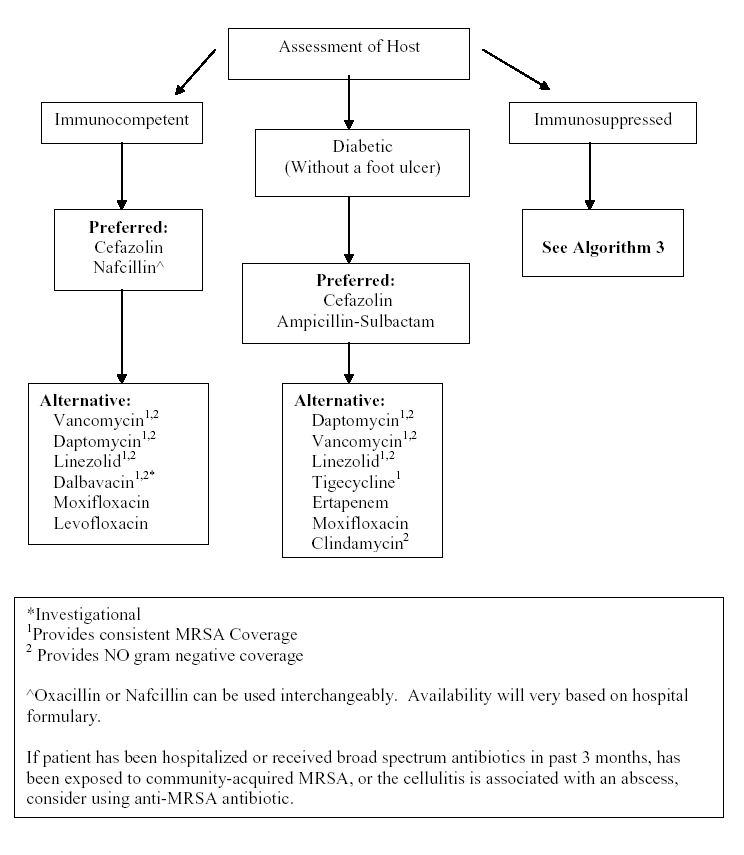
Algorithm 3: Empiric Intravenous Antibacterial Therapy for Cellulitis Based on Degree of Immunosuppression.
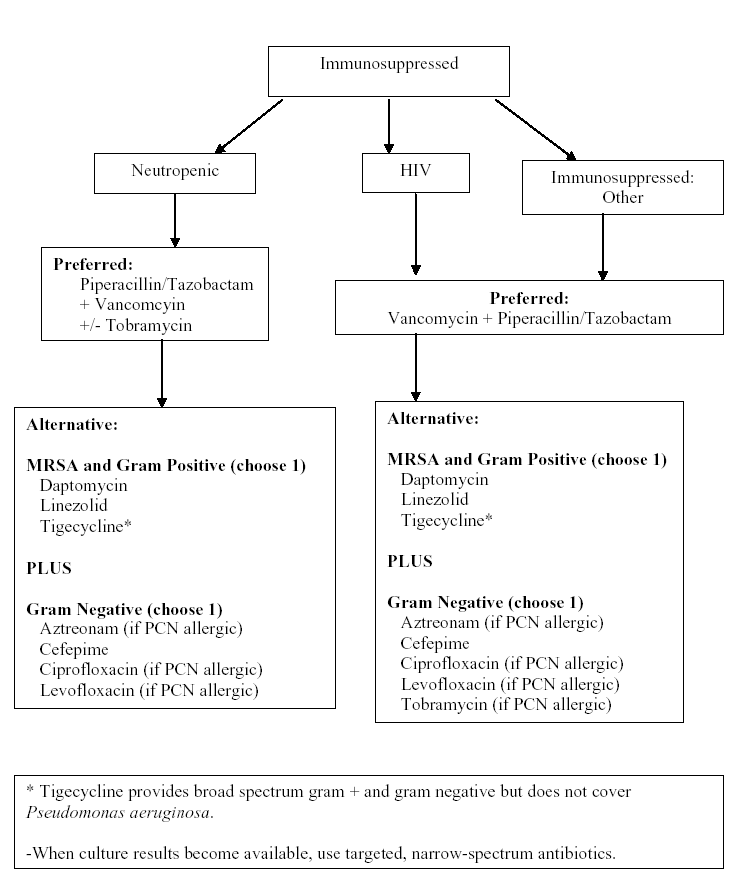
Algorithm 4: Empiric Antibacterial Agent Therapy Based on Type of Exposure.

Table 1: Specific Cellulitis Syndromes: Organisms and Empirical Therapy.
|
Syndrome |
Location |
Likely organisms |
Source |
Empiric parenteral therapy |
Oral regimens |
|
Abdominal wall cellulitis |
Abdominal wall, may extend to thighs |
Beta-hemolytic streptococci |
Morbid obesity, abdominal wall lymphedema |
Same as extremity cellulitis
|
Same as extremity cellulitis
|
|
Aquaculture cellulitis |
Varies |
Streptococcus iniae |
Fish |
Penicillin G but empiric coverage is same as extremity cellulitis |
Penicillin V but empiric coverage is same as extremity cellulitis
|
|
Bacterial cellulitis in the immunosuppressed patient |
Varies |
Group A streptococci, S aureus, P. aeruginosa, Serratia, Proteus, and the Enterobacteriaciae
|
Immunosuppression, bacteremia |
Cefepime OR imipenem OR piperacillin-tazobactam
In penicillin-allergic* [aztreonam + MRSA agent]
Consider the addition of tobramycin or ciprofloxacin to above until pathogen identified
In patients with possible MRSA: Same as extremity cellulitis with abscess |
Not recommended initially |
|
Dog and cat bite cellulitis |
Varies |
Pasteurella , S. aureus, streptococci, Capnocytophaga Bacteroides species, Fusobacterium, Porphyromonas species, Prevotella heparinolytica, Proprionibacterium, and Peptostreptococcus |
Oral organisms and skin flora |
Ampicillin-sulbactam OR ertapenem OR [clindamcyin + levofloxacin] OR [metronidazole + levofloxacin] |
Amoxicillin-clavulonate OR moxifloxacin OR [clindamycin + TMP/SX] OR [levofloxacin + metronidazole] |
|
Erysipelas |
Face and lower extremity |
Group A streptococci |
Antecedent streptococcal respiratory tract infection, skin ulcers, local trauma or abrasions, psoriatic or eczematous lesions |
Same as extremity cellulitis without abscess
|
Same as extremity cellulitis without abscess |
|
Extremity cellulitis with abscess |
Lower extremity |
MRSA |
Nasal colonization |
Daptomycin OR vancomycin OR linezolid |
TMP/SMZ OR doxycycline OR linezolid OR clindamycin |
|
Fresh water exposure cellulitis |
Varies |
Aeromonas hydrophilia |
Fresh water |
Levofloxacin OR cefepime OR carbapenems |
Same fluoroquinolones as listed for “parenteral” |
|
Human bite cellulitis |
Varies |
Normal oral flora of biter: Streptococci (especially viridans streptococci), S. aureus, Haemophilus, Eikenella and anaerobes |
Oral organisms and skin flora |
Same as dog and cat bite cellulitis |
Same as dog and cat bite cellulitis |
|
Meat handling cellulitis |
Hands |
Erysipelothrix rhusiopathiae |
Meat, poultry, hides, saltwater fish and shellfish |
Penicillin G OR ceftriaxone OR imipenem
If penicillin* allergic: levofloxacin OR clindamycin |
Penicillin V
If penicillin* allergic: ciprofloxacin OR clindamycin OR azithromycin |
|
Orbital cellulitis |
Orbital |
Streptococci, S. aureus, and non-spore-forming anaerobes |
Sinusitis, orbital trauma with fracture or foreign body, dacryocystitis, and infection of the teeth, middle ear, or face |
Same as preseptal cellulitis |
Same as preseptal cellulitis |
|
Perineal or post-gynecologic surgery cellulitis |
Abdominal wall, inguinal area, and/or the proximal thigh |
Non-group A beta-hemolytic streptococci, Staphylococcus aureus, enterococci, Escherichia coli, Peptostreptococcus, Prevotella and Porphyromonas, Bacteroides fragilis group, and Clostridium. |
Surgical procedures with local lymph node dissection and radiation for several types of gynecologic cancer |
Same as preseptal cellulitis |
Same as preseptal cellulitis |
|
Post-lumpectomy cellulitis |
Ipsilateral breast (may extend to shoulder, back, and arm) |
Non-group A beta-hemolytic streptococci |
Complication of surgeries which involve limited lymph node dissection and breast conservation and radiation |
Same as extremity cellulitis without abscess
|
Same as extremity cellulitis without abscess
|
|
Post-mastectomy cellulitis |
Ipsilateral arm |
Non-group A beta-hemolytic streptococci |
Complication of surgeries which involve lymph node dissection |
Same as extremity cellulitis without abscess
|
Same as extremity cellulitis without abscess
|
|
Post-saphenous venectomy cellulitis |
Lower extremity |
Beta-hemolytic streptococci |
Occur months to years after saphenous venectomy: Disruption of the cutaneous barrier, lymphedema, venous insufficiency |
Same as extremity cellulitis without an abscess
|
Same as extremity cellulitis without an abscess
|
|
Preseptal cellulitis |
Periorbital |
Streptococcus pneumoniae, Staphylococcus aureus, coagulase-negative Staphylococcus, and anaerobes, Haemophilus influenzae type b, S. pyogenes |
Contiguous infection of the soft tissues of the face and eyelids secondary to local trauma, insect bites, or foreign bodies |
[Ceftriaxone + metronidazole +/- vancomycin] OR [ertapenem +/- vancomycin] OR moxifloxacin |
Amoxicillin-clavulanate OR [levofloxacin + metronidazole] OR moxifloxacin
|
|
Saltwater exposure cellulitis |
Varies |
Vibrio species, particularly V. vulnificus |
Saltwater, ingestion of raw or undercooked seafood |
[Minocycline + cefotaxime] OR levofloxacin |
Minocycline + levofloxacin |
*Immediate-type hypersensitivity reaction
+ Nafcillin and oxacillin can be used interchangeably
Table 4: Indications for Inpatient Treatment of Cellulitis
|