Chronic Bronchitis (Exacerbations of Chronic Obstructive Pulmonary Disease)
Authors: Antonio Anzueto, M.D.
Several scientific organizations and the Global Initiative for Chronic Obstructive Lung Disease (GOLD) have proposed to define exacerbations of chronic obstructive pulmonary disease (COPD) as an event in the natural course of the disease characterized by a change in the patient’s baseline dyspnea, cough and/or sputum beyond day-to-day variability sufficient to warrant a change in management (10, 29, 36). These organizations have also proposed an operational classification of severity as: Level I: treated at home; Level II: requires hospitalization; and Level III: leads to respiratory failure. Various factors likely contribute to the acute exacerbations of COPD, including industrial pollutants, allergens, sedatives, congestive heart failure, and infections (viral and bacterial). The cause of an exacerbation may be multi-factorial, so that viral infection or levels of air pollution may exacerbate the existing inflammation in the airways, which in turn, may predispose to secondary bacterial infections (Table 1). It is estimated that bacterial infections play a part in between one-half and two-thirds of exacerbations (3, 10, 36).
Epidemiology
Acute exacerbations of chronic bronchitis (AECB) are a common cause of morbidity and mortality in this patient population (10, 36, 47). AECB is associated with frequent visits to physicians, up to 14 million doctor’s office visits and 600,000 hospitalizations (35, 43). COPD is the second leading cause of work disability (back pain is the leading cause) and is the third most frequent diagnosis for home-care services (20). The cost to treat COPD is around 24 billion dollars each year, including hospitalization costs and days off work. Significant numbers of hospitalized patients with acute exacerbations have modifiable risk factors including influenza vaccination, oxygen supplementations, smoking and occupational exposures (21, 22, 40). Several studies identified the risk factors associated with mortality in patients with AECB (11) (Table 2). AECB is associated with significant morbidity and mortality; 180-day mortality rate 33% and the two-year mortality rate 49% (11, 40).
These exacerbations also have major impact on the patients' quality of life. COPD patients are twice as likely as the general population to rate their health as being only fair or poor, nearly twice as likely to report recent limitations in their usual activities, and a large portion of them report frequent visits to their physician (39, 16). Studies have shown that exacerbation frequency is an important determinant of decline in lung function in COPD.
Relapse
Despite treatment with antibiotics, bronchodilators, and corticosteroids, up to 28% of patients discharged form the Emergency Department with acute exacerbations have recurrent symptoms within 14 days and 17% relapse and require hospitalization (2). The availability to identify patients who are at risk for relapse should improve decisions about hospital admissions and follow-up appointments. The risk factor for an exacerbation relapses are summarized in Table 3.
Role of Infection
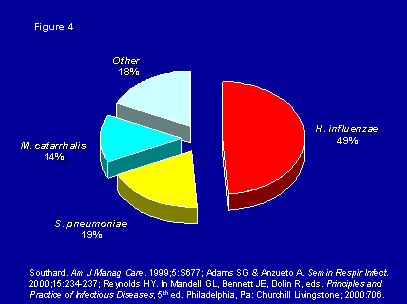
The role of bacteria in AECB is complex and takes into consideration several factors including the acquisition of new bacteria strains, changes in airway inflammation, and the ability of the host to overcome the infection (47). The most common bacteria associated with AECB are: Haemophilus influenzae, Haemophilus parainfluenzae, Moraxella catarrhalis, and Streptococcus pneumoniae (3, 6, 38); Atypical pathogens such as Mycoplasma pneumoniae and Chlamydia pneumoniaecan also be responsible for AECB (7) (Figure 1).
Patients with the most severe obstructive lung disease have a significantly higher prevalence of Gram-negative organisms such as Enterobacteriaceae and Pseudomonas species (17, 26). Patients were studied based on FEV1 (<50% versus <50% predicted). There were significantly larger numbers of H. influenzae and P. aeruginosa in the patients with FEV1 <50% of predicted (p<0.05). In contrast, there were significantly larger numbers of non-potentially pathogenic microorganisms in the group with FEV1 < 50% (p<0.05). H. influenzae was cultured significantly more commonly in patients who were actively smoking and whose FEV1 was <50% predicted. P. aeruginosa was also cultured significantly more frequently in those with poor lung function, FEV1<50% (26).
These bacterial pathogens can be isolated from sputum in an acute COPD exacerbation and during stable disease (28). During an exacerbation, 33% of the visits resulted in isolation of a new strain of a bacterial pathogen. Isolation of a new strain of H. influenzae, M. catarrhalis, or S. pneumoniae was associated with a significantly increased risk of an exacerbation (41). Thus the association between an exacerbation and the isolation of a new strain of a bacterial pathogen supports the causative role of bacteria in AECOPD.
DIAGNOSTIC PROCEDURES
Chest radiography and arterial blood gas sampling are useful in order to evaluate disease severity and to rule out pneumonia. Spirometric assessment at presentation or during treatment of acute exacerbation is not useful in judging the severity or guiding the management of the patient (3, 10, 36). Patient with recurrent exacerbations should have sputum sample collected for gram stain and culture in order to prescribe appropriate antimicrobial therapy.
TREATMENT
The objectives of treatment of AECB are: improve the patient’s symptoms; treat underlying infection if present; avoid additional invasive therapeutic maneuvers; increase the length of time between exacerbations (exacerbation-free interval); provide treatment as an outpatient; and decrease the need for hospitalization (3, 10, 36).
Antibiotic Resistance
Until the early 1980's, most bacteria species associated with acute exacerbation of chronic bronchitis could be assumed to be sensitive to ampicillin, erythromycin, tetracycline, and trimethoprim-sulfamethoxazole. These antibiotics were used for the management of these exacerbations, but in the 1990's the emergence of bacterial resistance has significantly compromised their use. Currently, 35% to 40% of Haemophilus influenzae and 95 - 100 % of the Moraxella catarrhalisisolates produced a beta-lactamase enzyme (15, 46). These microbes are resistant not only to ampicillin, but often resistant to erythromycin, trimethoprim-sulfamethoxazole and tetracycline (15, 46). There are also reports of the emergence ofpenicillin-resistant Streptococccus pneumoniae(PRSP). Data from surveillance studies have showed that in 2006 up to 35% PRSP; 24% were intermediately susceptible isolates and 10 – 15 % were highly resistant isolates (15, 46). The PRSP resistance is classified as high if the minimal inhibitory concentration (MIC) is more than 2 mc grams per ml. PRSP isolates are known to be also associated with decreased susceptibility to other antibiotics including cephalosporins, macrolides (clarithromycin (Biaxin®), erythromycin and azithromycin (Zithromax®), trimethoprim-sulfamethoxazole and tetracyclines. In the United States PRSP is not associated with decreased susceptibility to quinolones (15, 46). Risk factors that are present in patients that have infections with PRSP are summarized in (Table 5) (23).
Antibiotics
The specific etiology of acute exacerbation of COPD is difficult to determine. Sputum studies have significant limitations including the delay in obtaining the results, cost, and lack of sensitivity and specificity (3, 44). Scientific societies recommend antibiotic choices be based on local antibiotic susceptibilty patterns of the most common pathogens associated with acute exacerbation of COPD (10, 29, 36).
Many studies have demonstrated a benefit of antibiotics during an acute exacerbation, but not in preventing exacerbations (4, 5, 14, 34). Patients who are more likely to benefit from antibiotics are the ones that have all three clinical symptoms of an exacerbation (increased shortness of breath, increased sputum production, and a change in sputum purulence) at initial presentation. Overall, antibiotic-treated patients showed a more rapid improvement in peak flow and a greater percentage of clinical successes compared to those who received placebo.
There are additional potential benefits of antibiotic therapy for patients AECB. Antibiotics can reduce the burden of bacteria in the airway (19). 25% of stable COPD patients are colonized (usually <103 organisms) with potentially pathogenic bacteria (18, 27). However, a much larger percentage (50-75%) of patients with acute exacerbations have potentially pathogenic microorganisms in addition to significantly higher concentrations (frequently > 104 organisms) of bacteria in the large airways. The eradication of bacteria by antibiotics is thought to break the vicious cycle of infection, i.e., lung destruction leading to progression of the lung disease (19).
If the use of antibiotics to treat acute exacerbation of COPD has all the potential benefits discussed, does it matter which agent is chosen? The recommendations for what agent to use is based on the concept of risk-stratification of patients by clinical parameters and a targeted approach for the treatment of AECB (10, 36, 25). The classification of severity is based on patient’s presenting symptoms (Table 5). Selection of antibiotics based on these categories are summarize in Table 6.
Bronchodilators
Inhaled β-agonists and anticholinergic agents have been documented to decrease obstruction during an AECB (3, 9, 10, 12, 36, 24).
Corticosteroids
Systemic corticosteroids are indicated in the management of AECB (1, 3,10, 13, 32, 33, 36, 37, 45, 49). Clinical studies demonstrated that corticosteroids are associated with a faster improvement in FEV1, lower number of treatment failures, prolonged time to relapse, improved dyspnea, and shorter length of hospital stay. Prednisone treated patients experienced more side effects including increased appetite, weight gain, insomnia and were also more likely to experience hyperglycemia.
PREVENTION
The two most important prevention measures are smoking cessation and active immunizations, including influenza and pneumococcal vaccinations (10, 36). The frequency of lower respiratory infections, their morbidity and mortality are marked reduced with influenza vaccination (19, 30, 31). The polyvalent vaccine based on pneumococcal capsular serotypes have being shown to be effective in preventing pneumococcal bacteremia and pneumonia (8, 42). The pneumococcal and influenza vaccines can be given simultaneously immediately after an episode of pneumonia or acute exacerbation of COPD.
REFERENCES
1. Aaron SD, Vandemheen KL, Herbert P, Dales R, Stiell IG, Ahuja J, Dickerson G, Brison R, Rowe BH, Dreyer J, Yetisir E, Cass D, Wells G. Outpatient oral prednisone after emergency treatment of chronic obstructive pulmonary disease. N Eng J Med 2003;348:2618-2625. [PubMed]
2. Adams S, Melo J, Luther M, et al. Antibiotics are associated with lower relapse rates in outpatients with acute exacerbations of chronic obstructive pulmonary disease. Chest 2000; 117:1345-52 [PubMed]
3. Adams SG, Anzueto A. Treatment of acute exacerbations of chronic bronchitis. In: Antibiotics in Respiratory Infections (A. Anzueto, ED). Seminar Respir Infect 2000; 15:234-247 [PubMed]
4. Allegra L, Grassi C et al. Ruolo degli antibiotici nel trattamento delle riacutizza della bronchite cronica. Ital J Chest Dis 45:138-48, 1991.
5. >Anthonisen NR, Manfreda J, Warren CP, et al. Antibiotic therapy in acute exacerbation of chronic obstructive pulmonary disease. Ann Intern Med 1987; 106:196-04 [PubMed]
6. Ball P, Harris JM, Lowson D, et al. Acute infective exacerbations of chronic bronchitis. QJM 1995; 88:61-8 [PubMed]
7. Blasi F, Damato S, Cosentini R, Tarsia P, Raccanelli R, Centanni S, Allegra L. Chlamydia pneumoniae and chronic bronchitis: association with severity and bacterial clearance following treatment. Thorax 2002;57(8):672-676. [PubMed]
8. Butler JC, Breiman RF, Campbell JF, Lipman HB, Broome CV, and Facklam RR. Pneumococcal polysaccharide vaccine efficacy. An evaluation of current recommendations. JAMA 1993; 270:1826-31. [PubMed]
9. Carrera M, Sala E, Cosio BG, Agusti AG. Hospital treatment of chronic obstructive pulmonary disease exacerbation: an evidence-based review. Arch Bronchoneumol 2005; 41:220-229. [PubMed]
10. Celli BR, MacNee W. Standards for the diagnosis and treatment of patients with COPD: a summary of the ATS/ERS position paper. Eur Respir J. 2004;23:932-946. [PubMed]
11. Connors AF Jr, Dawson NV, Tomas C, et al. Outcomes following acute exacerbation of severe chronic obstructive lung disease. The SUPPORT investigators (Study to Understand Prognoses and Preferences for Outcomes and Risks of Treatment). Am J Respir Crit Care Med 1996; 154:959-67 [PubMed]
12. Cydulka RK, Rowe BH, Clark S, Emerman CL, Camargo CA Jr; MARC Investigators. Emergency department management of acute exacerbationis of chronic obstructive pulmonary disease in the elderly: the Multicenter Airway Research Consortium. J Am Geriatr Soc 2003;51:908-916. [PubMed]
13. Davies L, Angus R, Calverley P. Oral corticosteroids in patients admitted to hospital with exacerbations of chronic obstructive pulmonary disease: a prospective randomised controlled trial. Lancet 1999;354:456-460. [PubMed]
14. Dimipoulos G, Siempos II, Korbila IP, Manta KG, Falgas ME. Comparison of first-line with second-line antibiotics for acute exacerbations of chronic bronchitis. A Meta-analysis of randomized controlled trials. Chest 2007; 132: 4447–4455.[PubMed]
15. Doern GV, Richter SS, Miller A, Miller N, Rice C, Heilman K, Beekmann S. Antimicrobial resistance among Streptococcus pneumonia in the United States: Have we begun to turn the corner on resistance to certain antimicrobial classes. Clin Inf Dis 2005; 41:139-148. [PubMed]
16. Donaldson GC, Seemungal TAR, Bhomik A, Wedzicha JA. Relationship between exacerbation frequency and lung function decline in chronic obstructive pulmonary disease. Thorax 2002;57: 847-852. [PubMed]
17. Eller J, Ede A, Schaberg T, et al. Infective exacerbations of chronic bronchitis: relation between bacteriologic aetiology and lung function. Chest 1998; 113:1542-48. [PubMed]
18. Gompertz S, O’Brien C, Bayley DL, Hill SL, Stockley RA. Changes in bronchial inflammation during acute exacerbations of chronic bronchitis. Eur Respir J 2001; 17:1112-19. [PubMed]
19. Gross PA, Hermogenes AW, Sacks HS, Lau J, and Levandowski RA. The efficacy of influenza vaccine in elderly persons. A meta-analysis and review of the literature. Ann Intern Med 1995; 123:518-27. [PubMed]
20. Healthcare Cost and Utilization Project. 1997 Nationwide Inpatient Sample. Agency for Healthcare Research and Policy. Available at: www.ahcpr.gov/data/hcup/hcupnet.htm. [PubMed]
21. Lindenauer PK, Pekow P, Gao S, Crawford AS, Gutierrez B, Benjamín EM. Quality of care for patients hospitalized for acute exacerbations of chronic obstructive pulmonary disease. Ann Int Med 2006;144:894-903. [PubMed]
22. MacNee W. Acute exacerbations of COPD. Swiss Med Wkly 2003;133:247-257. [PubMed]
23. Mandell LA, Wunderink RG, Anzueto a, etl al. Infectious Disease Society of America/American thoracic Society Consensus Guidelines on the management of Community Acquired Pneumonia in Adults. Clin Inf Dis 2007; 44:S27-72.[PubMed]
24. McCrory D, Brown C. Anticholinergic bronchodilators versus beta2-sympathomimetic agents for acute exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2006.
25. Meyer B, La Forge J, Low DE et al. Canadian Guidelines for the management of acute exacerbations of Chronic bronchitis: executive summary. Can Respir J 2003; 10:248-58. [PubMed]
26. Miravitles M, Espinosa C, Fernandez-Laso E, et al. Relationship between bacterial flora in sputum and functional impairment in patients with acute exacerbations of COPD. Chest 1999; 116:40-6. [PubMed]
27. Monsó JR, Rosell A, Manterola J, et al. Bacterial infection in chronic obstructive pulmonary disease. Study of stable and exacerbated outpatients using the protected specimen brush. Am J Respir Crit Care Med 1995; 152:1316-20. [PubMed]
28. Murphy TF, Sethi S. Bacterial infection in chronic obstructive pulmonary disease. Am Rev Respir Dis 1992;146:1067-1083. [PubMed]
29. National Institute for Clinical Excellence (NICE) Chronic obstructive pulmonary disease: national clinical guideline on management of chronic obstructive pulmonary disease in adults in primary and secondary care. Thorax, 2004. 59, Suppl 1: 1-232.
30. Nichol KL, Baken L, Nelson A. Relation between Influenza Vaccination and Outpatient Visits, Hospitalization, and Mortality in Elderly Persons with Chronic Lung Disease Ann Intern Med1999; 130:397-403 [PubMed]
31. Nichol KL, NNOrdin JD, Nelson DB et al. Effectiveness of Influenza Vaccine in Community-Dwelling Elderly. N Engl J Med 2007; 357:1373-1381. [PubMed]
32. Niewoehner D. The role of systemic corticosteroids in acute exacerbation of chronic obstructive pulmonary disease. Am J Respir Med 2002:1:243-248. [PubMed]
33. Niewoehner DE, Erbland ML, Deupree RH, Collins D, Gross NJ, Light RW, Anderson P, Morgan NA. Effect of sytemic glucocorticoids on exacerbations of chronic obstructive pulmonary disease. Department of Veterans Affairs Cooperative Study Group. N Eng J Med 1999;304:1941-1947. [PubMed]
34. Nouira S, Marghli S, Belghith M, et al. Once daily oral ofloxacin in chronic obstructive pulmonary disease exacerbation requiring mechanical ventilation: a randomized placebo-controlled trial. Lancet 2001;358:2020-2025. [PubMed]
35. Peters DK, Kochanek DK, Murphy SL. Deaths: final data for 1996. Natl Vital Stat Rep 1998; 47:1-100.
36. Rabe K, Hurd S, Anzueto A, et al. Global Initiative for Chronic Obstructive Lung Disease. Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease. GOLD Executive Summary. Amer J Respir Crit Care Med 2007; 176: 532-555. [PubMed]
37. Sayiner A, Aytemur ZA, Cirio M, Unsal I. Systemic glucocorticoids in severe exacerbations of COPD. Chest 2001;119:726-730.[PubMed]
38. Seemugal T, Harper-Owen R, Bhowmik A, Moric I, Sanderson G, Message S et al. Respiratory viruses, symptoms and inflammatory markers in acute exacerbations and stable chronic obstructive pulmonary disease. Am J Repir Crit Care Med 2001; 164:1618-23. [PubMed]
39. Seemungal TA, Donaldson GC, Bhowmik A, Jeffries DJ, Wedzicha JA. Time course and recovery of exacerbations in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2000;161 1608-1613. [PubMed]
40. Seneff MG, Wagner DP, Wagner RP, et al. Hospital and 1-year survival of patients admitted to intensive care units with acute exacerbation of chronic obstructive pulmonary disease. JAMA 1995; 274:1852-7. [PubMed]
41. Sethi S, Evans N, Grant BJB, Murphy TF. New strains of bacteria and exacerbation s of chronic obstructive pulmonary disease. NEJM 2002; 347:465-471. [PubMed]
42. Sisk JE, Whang W, Butler JC, Sneller VP, and Whitney CG. Cost-effectiveness of vaccination against invasive pneumococcal disease among people 50 through 64 years of age: role of comorbid conditions and race. Ann Intern Med 2003; 138:960-8. [PubMed]
43. Statistical Abstract of the United Statess 1997. U.S. Department of Commerce, Bureau of the Census. Washington, DC. U.S. Department of Commerce, 1997.
44. Stockley RA, O’Brien C, Pye A, et al. Relationship of sputum color to nature and outpatient management of acute exacerbations of COPD. Chest. 2000;117:1638-1645. [PubMed]
45. Thompson WH, Nelson Cp, Carvalho P, Charan NB, Crowley JJ. Controlled trial of oral prednisone in outpatients with acute COPD exacerbation. Am J Respir Crit Care Med 1996;154:407-412. [PubMed]
46. Thronsberry C, Ogilvie P, Kahn J et al. Surveillance of antimicrobial resistance in Streptococcus pneumonia, Haemophilus influenzae, and Moraxella catarrhalis in the United States in 1996 - 1997 respiratory season. Diag Microbiol Infec Dis 29:249-257, 1997. [PubMed]
47. Veeramachaneni SB, Sethi S. Pathogenesis of bacterial exacerbations of COPD. COPD: J Chronic Obstructive Pul Dis 2006;3:109-115. [PubMed]
48. Wilkinson TM, Donaldson GC, Hurst JR, Seemungal TA, Wedzicha JA. Early therapy improves outcomes of exacerbations of chronic obstructive pulmonary disease. Am J Resp Crit Care Med 2004;169:1298-1303. [PubMed]
49. Wood-Baker R, et al., Systemic corticosteroids for acute exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev, 2006. [PubMed]
Tables
Table 1: The Most Common Causes of Acute Exacerbation of COPD (AECB)
| Common | |||
|---|---|---|---|
| Environmental conditions | |||
| Infec |
- Viral : | Rhinovirus sp, influenza | |
| - Bacteria : | H. influenzae, .S pneumonia, M catharrhalis, Enterobacteraceas sp., Pseudomonas sp. | ||
| Other | |||
| No influenza vaccinations | |||
| Non-compliance with long-term oxygen therapy | |||
| |
|||
| Occupational exposures |
|||
| Non pulmonary rehabilitation | |||
(References 3, 10, 36)
Table 2: Predictors of Mortality in Patients with AECB
|
(From references 11,40)
Table 3: Risk Factor for AECB Relapse
|
(From references 2,3,10)
Table 4: Clinical Risk Factors Associated with Penicillin Resistant and Multidrug Resistant Streptococccus pneumoniae.*
|
* These factors have being identified in patients with community acquired pneumonia (23).
Table 5: Patient Profiles from the Canadian Chronic Bronchitis Guidelines
Acute bronchitis (Group 1) Healthy people without previous respiratory problems |
“Simple” chronic bronchitis (Group 2) Age £ 65 years old and < 4 exacerbations per year and Minimal or no impairment in pulmonary function and No co-morbid conditions |
“Complicated” chronic bronchitis (Group 3) Age > 65 years old or FEV1 < 50% predicted or ³ 4 exacerbations per year |
“Complicated” chronic bronchitis with co-morbid illness (Group 4) Above criteria for Group 3, plus: Congestive heart failure or Diabetes or Chronic renal failure or Chronic liver disease or Other chronic disease |
Adapted from Balter MS, et al (25)
Table 6 : Association Between Classification of Severity, Probably Pathogens and Recommended Antibiotic Therapy
Category |
Probable Pathogen |
Therapy |
|---|---|---|
Acute Bronchitis (Group 1) |
Viral |
Symptomatic |
"Simple" AECOPD (Group 2) |
Haemophilus spp.(H. influenzae),M. catarrhalis, S. pneumoniae, Atypical organisms (possibly) |
Doxycycline or macrolide (azithromycin/clarithromycin) orcephalosporins. Respiratory Fluoroquinolones * |
"Complicated" AECOPD (Groups 3 & 4) |
As above, with the possible addition of Pseudomonas spp, Enterobacteriaceae, & other Gram negative organisms |
Respiratory Fluoroquinolones * * |
* Consider in patients with risk factors for resistant pathogens.
** If at risk for Pseudomonas infection, use Ciprofloxacin or high dose levofloxacin..
lang="da" xml:lang="da">Adapted from Balter MS, et al (25).
Figure 1: Bacterial etiologies of acute exacerbations of chronic bronchitis
What's New
Babu Suresh K, et al. Role of long term antibiotics in chronic respiratory diseases. Respir Med 2013 Epub ahead of pub.
Wenzel RP, et al. Antibiotic prevention of acute exacerbations of COPD. N Engl J Med 2012;367:340-347.
Nouira S, et al. Standard Versus Newer Antibacterial Agents in the Treatment of Severe Aacute Exacerbation of Chronic Obstructive Pulmonary Disease: a Randomized Trial of Trimethoprim-Sulfamethoxazole Versus Ciprofloxacin. Clin Infect Dis. 2010 Jul 15;51:143-9.
