The Influenza Pandemic of 1918:
The Medical and Scientific Conceptions of Influenza
Molly Billings and Jeremy Schneider

Scientific ideas about influenza, the disease and its origins, shaped the public health and medical responses . In 1918 infectious diseases were beginning to be unraveled. Pasteur and Koch had solidified the germ theory of disease through clear experiments and clever science. The bacillus responsible for many infections such as tuberculosis and anthrax had been visualized, isolated and identified. Koch's postulates had been developed to systematically and definitively link a disease to a specific microbial agent. The petri dish was widely used to grow sterile cultures of bacteria and investigate bacterial flora. Vaccines had been created for bacterial infections and even the unseen rabies virus by serial passage techniques. The immune system was explained by Paul Erhlich and his side-chain theory. Tests of antibodies such as Wasserman and coagulation experiments were becoming commonplace. Science and medicine were on their way to their complete entanglement and fusion as scientific principles and methodologies made their way into clinical practice, diagnostics and therapy.
The Clinical Descriptions of Influenza
 Patients with the influenza disease of the epidemic
were generally characterized by common
complaints associated with the flu. They
had body aches, muscle and joint pain,
headache, a sore throat and a
unproductive cough with occasional harsh
breathing (JAMA, 1/25/1919). The most
common sign of infection was the fever,
which ranged from 100 to 104 °F and
lasted for a few days. The onset of the
epidemic influenza
was peculiarly sudden, as people were
struck down with dizziness, weakness and
pain while on duty or in the street
(BMJ, 7/13/1918). After the disease was
established the mucous membranes became
reddened with sneezing. In some cases
there was a hemorrhage of the mucous
membranes of the nose and bloody noses
were commonly seen. Vomiting occurred on
occasion. Sometimes patients experienced
diarrhea, but, more commonly, they
suffered from constipation (JAMA,
10/3/1918). A few physicians associated
psychoses with influenza
infection. One article says that "the
frequency of mental disturbances
accompanying the acute illness in the
epidemic has been the subject of
frequent comment," (JAMA, 1/25/1919) The
danger of an influenza
infection was its tendency to progress
into the often fatal pneumonia caused by
secondary bacterial infection. In the
patients that did not rapidly recover
after three or four days of fever, an
"irregular pyrexia" due to bronchitis or
broncopneumonia was often observed (BMJ,
7/13/1918). The pneumonia would often
appear after a period of normal
temperature with a sharp spike and
expectorant of bright red blood. The
lobes of the lung became speckled with
"pneumonic consolidations." The fatal
cases developed toxemia and vasomotor
depression (JAMA, 10/3/1918). It was
this tendency for secondary
complications that made this
influenza
infection so deadly.
Patients with the influenza disease of the epidemic
were generally characterized by common
complaints associated with the flu. They
had body aches, muscle and joint pain,
headache, a sore throat and a
unproductive cough with occasional harsh
breathing (JAMA, 1/25/1919). The most
common sign of infection was the fever,
which ranged from 100 to 104 °F and
lasted for a few days. The onset of the
epidemic influenza
was peculiarly sudden, as people were
struck down with dizziness, weakness and
pain while on duty or in the street
(BMJ, 7/13/1918). After the disease was
established the mucous membranes became
reddened with sneezing. In some cases
there was a hemorrhage of the mucous
membranes of the nose and bloody noses
were commonly seen. Vomiting occurred on
occasion. Sometimes patients experienced
diarrhea, but, more commonly, they
suffered from constipation (JAMA,
10/3/1918). A few physicians associated
psychoses with influenza
infection. One article says that "the
frequency of mental disturbances
accompanying the acute illness in the
epidemic has been the subject of
frequent comment," (JAMA, 1/25/1919) The
danger of an influenza
infection was its tendency to progress
into the often fatal pneumonia caused by
secondary bacterial infection. In the
patients that did not rapidly recover
after three or four days of fever, an
"irregular pyrexia" due to bronchitis or
broncopneumonia was often observed (BMJ,
7/13/1918). The pneumonia would often
appear after a period of normal
temperature with a sharp spike and
expectorant of bright red blood. The
lobes of the lung became speckled with
"pneumonic consolidations." The fatal
cases developed toxemia and vasomotor
depression (JAMA, 10/3/1918). It was
this tendency for secondary
complications that made this
influenza
infection so deadly.

A military hospital ward in 1918
In the medical literature characterizing the influenza disease, new diagnostic techniques were frequently used to describe the clinical appearance. The most basic clinical guideline was the temperature, a record of which was kept in a table over time. Also closely monitored was the pulse rate. One clinical account said that "the pulse was remarkably slow," (JAMA, 4/12/1919) while others noted that the pulse rate did not increase as expected. Additionally, the respiration rate was measured and reported to provide clues of the clinical progression. Patients were also occasionally "roentgenographed" or chest x-rayed (JAMA, 1/25/1919). The discussion of clinical influenza also often included analysis of the blood. The number of white blood cells were counted for many patients; leukopenia was commonly associated with influenza. The albumin was also measured via urine analysis, since it was noted that transient albuminuria was frequent in influenza patients. The Wassermann reaction was a new test for antibodies in blood which was utilized in diagnosis and monitoring of the infection (JAMA, 10/3/1918). These new scientific measurements enabled physicians to record precisely the progress of the influenza infection and better predict its outcome.
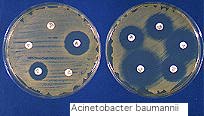
The most novel of these tests were the blood and sputum cultures. Building on the germ theory of disease, the physicians and their associated research scientists attempted to find the culprit for this deadly infection. Physicians would commonly order both blood and sputum cultures of their influenza and pneumonia patients mostly for research and investigative purposes. During an influenza epidemic at Camp Lewis, a military training camp,"in all cases of pneumonia...a sputum study, white blood and differential count, blood culture and urine examinations were made as routine," (JAMA, 1/25/1919). The bacterial flora of the nasopharynx of some patients was also cultured, since droplets were responsible for much of the dissemination of the infection. The collected swabs and specimens were inoculated onto blood agar of petri dishes. The bacterial colonies which subsequently grew were closely studied to find the causal organism. Commonly found were pneumococcus, streptococcus, staphylococcus and Bacillus influenzae (JAMA, 4/12/1919). These new laboratory tests used in the clinical setting brought a solid scientific, biological basis to the practice of medicine. Medicine had become fully scientific and technologic in its understanding and characterization of the influenza epidemic.
Treatment and Therapy
The therapeutic remedies for influenza patients varied from the newly developed drugs to oils and herbs. The therapy was much less scientific than the diagnostics, as the drugs had no clearly explicable theory of action. The treatment was largely symptomatic, aiming to reduce fever or pain. Aspirin, or acetylsalicylic acid, was a common remedy. For secondary pneumonia, doses of epinephrin were given. To combat the cyanosis physicians gave oxygen by mask or some injected it under the skin (JAMA, 10/3/1918). Others used salicin which reduced pain, discomfort and fever and claimed to reduce the infectivity of the patient. Another popular remedy was cinnamon in powder or oil form with milk to reduce temperature (BMJ, 10/19/1918). Finally, salt of quinine was suggested as a treatment. Most physicians agreed that the patient should be kept in bed (BMJ, 7/13/1918) and advised plenty of fluids and nourishment. The application of cold to the head, with warm packs or warm drinks was also advised. Warm baths were used as a hydrotherapeutic method in hospitals but were discarded for lack of success (JAMA, 10/3/1918). These treatments, like the suggested prophylactic measures of the public health officials, seemed to originate in the common social practices and not in the growing field of scientific medicine. It seems that as science began to enter the medical field, it served only for explanatory, diagnostic and preventative measures such as technical tests and vaccines. This science had little use once a person was ill.
 However, a few proposed treatments did
incorporate scientific ideas of germ
theory and the immune system. O'Malley
and Hartman suggested treating
influenza
patients with the serum of convalescent
patients. They theorized that the
antibodies would boost the immune system
of sick patients. Another recommended
treatments was "digitalis," the
intravenous administration of isotonic
glucose and sodium bicarbonate,
practiced primarily in military camps
(JAMA, 1/4/1919). Ross and Hund also
utilized ideas about the immune system
and properties of the blood to
neutralize toxins and circulate white
blood cells. They believed that the best
treatment for
influenza should
aim to: "...neutralize or render the
intoxicant inert...and prevent the blood
destruction with its destructive
leukopenia and lessened coagulability,"
(JAMA, 3/1/1919). They tried to create a
therapeutic immune serum to fight
infection. These therapies built on
current scientific ideas and represented
the highest biomedical, technological
treatments.
However, a few proposed treatments did
incorporate scientific ideas of germ
theory and the immune system. O'Malley
and Hartman suggested treating
influenza
patients with the serum of convalescent
patients. They theorized that the
antibodies would boost the immune system
of sick patients. Another recommended
treatments was "digitalis," the
intravenous administration of isotonic
glucose and sodium bicarbonate,
practiced primarily in military camps
(JAMA, 1/4/1919). Ross and Hund also
utilized ideas about the immune system
and properties of the blood to
neutralize toxins and circulate white
blood cells. They believed that the best
treatment for
influenza should
aim to: "...neutralize or render the
intoxicant inert...and prevent the blood
destruction with its destructive
leukopenia and lessened coagulability,"
(JAMA, 3/1/1919). They tried to create a
therapeutic immune serum to fight
infection. These therapies built on
current scientific ideas and represented
the highest biomedical, technological
treatments.
The Etiology of Influenza in 1918
During the 1890 influenza epidemic, Pfeiffer found what he determined to be the microbial etiological agent of influenza. In the sputum and respiratory tract of influenza patients in 1892, he isolated the bacteria Bacillus influenzae , which was accepted as the true "virus," though it was not found in localized outbreaks (BMJ, 11/2/1918). However, in studies of the 1907-8 epidemic in the US, Lord had found the bacillus in only 3 of 20 cases. He also found the bacillus in 30% of cultures of sputum from TB patients. Rosenthal further refuted the finding when he found the bacillus in 1 of 6 healthy people in 1900 (JAMA, 1/18/1919). The bacillus was also found to be present in all cases of whooping cough and many cases of measles, chronic bronchitis and scarlet fever (JAMA, 10/5/1918). The influenza pandemic provided scientists with the opportunity to confirm or refute this contested microbe as the cause of influenza. The sputum studies from the Camp Lewis epidemic found only a few influenza cases harvesting the influenza bacilli and most contained type IV pneumococcus . They concluded that "the recent epidemic at Camp Lewis was an acute respiratory infection and not an epidemic due to Bacillus influenzae ," (JAMA, 1/25/1919). This finding along with others suggested to most scientists that the Pfeiffer's Bacillus was not the cause of influenza.
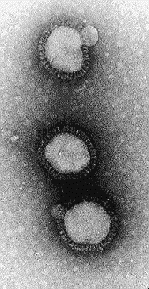
During the 1918-19 influenza pandemic, there was a great drive to find the etiological agent responsible for the deadly scourge. Scientists in their labs were working hard, using the cultures obtained from clinics, to isolate the etiological agent for influenza. As a report early in the epidemic said, "the 'influence' of influenza is still veiled in mystery, " (JAMA, 10/5/1918). The nominated bacillus influenzae bacteria seemed to be the wrong culprit and scientists scrambled to isolate the true cause. In the journals, many authors speculated on the type of agent -- was it a new microbe, was it a bacteria, was it a virus ? One journal offered that "the severity of the present pandemic, the suddenness of onset...led to the suggestion that the disease cannot be influenza but some other and more lethal infection," (BMJ, 11/2/1918). However, most accepted that the epidemic disease was influenza based on the familiar symptoms and known pattern of disease. The respiratory disease of influenza was understood to give warning in the late spring of its potential effects upon its recrudescence in the winter (BMJ, 10/19/1918). One article with foresight stated that "there can be no question that the virus of influenza is a living organism...it is possibly beyond the range of microscopic vision," (BMJ, 11/16/1918). Another article confirmed the idea of an "undiscovered virus" and noted that pneumococci and streptococci were responsible for "the gravity of the secondary pulmonary complications," (BMJ, 11/2/1918). The article went on to offer the idea of a symbiosis of virus and secondary bacterial infection combining to increase the severity of the disease.
In their attempts to find the responsible agent for the influenza pandemic, investigators were developing ideas of infectious microbes and the concept of the virus. The idea of the virus as an infectious agent had been around for years. The articles of the period refer to the "virus" in their discussion but do not consistently use it to be an infectious microbe, distinctive from bacteria. The term virus has the same usage and application as bacillus. In 1918, a virus was defined scientifically to be a submicroscopic infectious entity which could be filtered but not grown in vitro . In the 1880s, Pasteur developed an attenuated vaccine for the rabies virus by serial passage. Ivanoski's work on the tobacco mosaic virus in 1890s lead to the discovery of the virus. He found an infectious agent that acted as a micro-organism as it multiplied, yet passed through the sterilizing filter as a non-microbe. By the 1910s, several viruses, defined as filterable infectious microbes, had been identified as causing infectious disease (Hughes). However, the scientists were still conceptually behind in defining a virus; they distinguished it only by size from a bacteria and not as a pathogen with a distinct life cycle dependent on infection of a host cell.
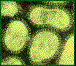
Experiments by Nicolle and Le Bailly in Paris were the earliest suggestions that influenza was caused by a "filter-passing virus," (BMJ, 11/2/1918). They filtered out the bacteria from bronchial expectoration of an influenza patient and injected the filtrate into the eyes and nose of two monkeys. The monkeys subsequently developed fevers and marked depression. The filtrate was later administered subcutaneously to a human volunteer, who developed typical signs of influenza. They reasoned that the inoculated person developed influenza from the filtrate since no one else in their quarters developed influenza (JAMA, 12/28/1918). These scientists followed Koch's postulates as they isolated the causal agent from patients with the illness and used it to reproduce the same illness in animals. Through these studies, the scientists proved that influenza was caused by a submicroscopic infectious agent and not a bacteria, refuting the claims of Pfeiffer and advancing the field of virology. They were on their way to discerning the virus and characterizing the orthomyxo viruses that lead to the disease of influenza.
![]()
These scientific experiments had immediate preventative applications, assisting in the effort to create a effective vaccine to prevent influenza. This was the ultimate goal of most studies, since vaccines were thought to be the best preventative solution in the early 20th century. Several experiments attempted to produce vaccines, each with a different understanding of the etiology of fatal influenza infection. A Dr. Rosenow invented a vaccine to target the multiple bacterial agents found in the serum of patients. He aimed to raise immunity against the bacteria, the "common causes of death," and not the cause of the initial symptoms, by inoculating with the proportions found in the lungs and sputum (JAMA, 1/4/1919). The vaccines made for the British forces took a similar approach and were "mixed vaccines" of pneumococcus and lethal streptococcus. The vaccine development therefore focused on the culture results of what could be isolated from the sickest patients and lagged behind the scientific progress.