Thrombocytopenia
Authors: Satheesh K. Kathula, M.D., F.A.C.P.
Definition
A platelet count of less than the lower normal range for a particular lab (generally the normal platelet count for most laboratories is 130,000 to 400,000/mcL). For practical purposes, one should consider a platelet count of <100,000/mcL as a definition of thrombocytopenia.
Pathogenesis and Mechanism
Thrombocytopenia is caused by several mechanisms. The two most common ones are
decreased production in the bone marrow and increased destruction of platelets
(immune thrombocytopenia purpura, drug induced, etc) in the peripheral blood.
Thrombocytopenia due to dilution can occur in patients receiving multiple
transfusions or in pregnant women as a result of increased plasma volume.
Platelets are consumed in hypersplenism and disseminated intravascular
coagulation. Pseudo or spurious thrombocytopenia is a relatively common cause of
thrombocytopenia due to EDTArelated platelet clumping ![]() . Review of peripheral
smear is diagnostic.
. Review of peripheral
smear is diagnostic.
Etiology
HIV and Thrombocytopenia:
About 40% of HIV patients have some degree of thrombocytopenia. In 10% of patients, low platelet count may be the initial manifestation. Primary HIV associated thrombocytopenia is the most common cause, due to increased destruction and ineffective production of platelets. Primary HIV associated thrombocytopenia may also be indistinguishable from immune thrombocytopenia purpura. Some HIV positive patients may have splenomegaly with subsequent platelet sequestration. The etiologies of thrombocytopenia in HIV are listed in Table 4.
Sepsis and Thrombocytopenia:
Thrombocytopenia occurs in up to 20-35% of patients admitted to intensive care unit. Sepsis is responsible for half of these. There are several mechanisms involved: bone marrow suppression, EDTA related platelet clumping (pseudo thrombocytopenia), immune and non-immune disseminated intravascular coagulation destruction/consumption of platelets. There is an inverse relationship between the severity of sepsis and the platelet count. Thrombocytopenia is an independent risk factor for mortality in patients with sepsis.
Disseminated Intravascular Coagulation:
Disseminated intravascular coagulation results from injury to vascular endothelium, leading to exposure of tissue factor, which activates the extrinsic factor pathway in coagulation cascade. In this process, consumption of the coagulation factors and platelets leads to bleeding, hence the name consumptive coagulopathy. Several factors trigger disseminated intravascular coagulation, including sepsis, malignancy, extensive trauma/burns, intrauterine fetal death, etc. Prolonged prothrombin time and activated partial thromboplastin time, low fibrinogen, increased D-dimer, thrombocytopenia are all suggestive but not diagnostic. There is no specific treatment for disseminated intravascular coagulation other than addressing the underlying problem. Transfusion of blood products such as cryoprecipitate and platelets should be considered only if there is significant bleeding.
Thrombotic Thrombocytopenic Purpura:
This is a potentially life threatening entity which can be treated very effectively with total plasma exchange. Thrombotic thrombocytopenic purpura is thought to stem from deficiency of von Willibrand factor cleaving enzyme also known metaloprotease. It manifests as thrombocytopenia, microangiopathic hemolytic anemia (increased reticulocyte count, LDH, low haptoglobin and presence of fragmented red blood cells on blood smear), altered mental status, renal failure and fevers (the so called ‘pentad’). Unfortunately, there is no diagnostic test for thrombotic thrombocytopenic purpura. Presence of thrombocytopenia, microangiopathic hemolytic anemia with any of the aforementioned features is highly indicative of thrombotic thrombocytopenic purpura.
Immune Thrombocytopenic Purpura (TTP):
Immune thrombocytopenic purpura is usually idiopathic and occasionally may be secondary to an auto-immune process such as lupus, rheumatoid arthritis, or lymphoproliferative disorders (lymphomas or chronic lymphocytic leukemia). Infection with HIV, hepatitis B and C and helicobacter pylori may also be associated with immune thrombocytopenic purpura. Bleeding is rare despite severely low platelet count due to the presence of functional platelets. It is usually a diagnosis of exclusion. Presence of adequate or increased number of megakaryocytes in the bone marrow with no other explanation confirms immune thrombocytopenic purpura. The initial treatment is typically steroids. Intravenous immunoglobulin, rituximab, and splenectomy are other treatment modalities.
Hemolysis (Elevated Liver Enzymes and Low Platelets (HELLP) Syndrome):
HELLP is exclusive to pregnancy, and is an extreme form of pre-eclampsia. Although it typically occurs in third trimester, it can be seen in any time of pregnancy. Clinical manifestations include pain in the right upper quadrant, high blood pressure, thrombocytopenia, and elevated liver enzymes. Delivery is the treatment of choice.
Heparin Induced Thrombocytopenia:
This is a life threatening condition caused by exposure to either unfractionated or low molecular heparin. It is caused by the formation of antibodies against heparin and platelet factor 4 antibody complex. It occurs 5 days after the exposure to heparin, unless the patient has previously been exposed to heparin. Patients present with thrombocytopenia and venous or arterial thrombosis. Diagnosis is made by either serologic or functional assays. Heparin must be stopped if there is a clinical suspicion and a direct thrombin inhibitor (lepirudin, argatroban, etc.) must be started immediately even if there is no thrombosis.
A complete list of the various causes of thrombocytopenia is available in Table 1, Table 2, Table 3.
Clinical Manifestations
There is no strong correlation between the severity of bleeding and the number of platelets. Multiple factors play a role. A patient with immune thrombocytopenic purpura may not bleed even if the platelet count is < 10,000/mcl due to very functional platelets. On the other hand, a patient with mild thrombocytopenia may develop significant bleeding if he/she is on medications like heparin, aspirin or pentoxyfilline. Renal failure sepsis, coagulopathy from any cause can be contributory as well. The common clinical presentations of thrombocytopenia are listed in Table 5. Serious bleeding such as spontaneous intracranial bleeding is very rare unless the platelet count is less than 10,000/mcL
Diagnosis
Step 1: Review complete blood count (CBC) carefully. High mean platelet volume or mean platelet volume (MPV) (like mean corpuscular volume (MCV) for red blood cells) indicates large platelets, which occurs in pseudo thrombocytopenia, peripheral destruction of platelets or splenic sequestration. Isolated thrombocytopenia is usually a sign of immune thrombocytopenic purpura. Presence of simultaneous leucopenia and anemia indicate a generalized process such as bone marrow problems, cyanocobalmine or folate deficiency or hypersplenism. High MCV may suggest B12 or folate deficiency, alcohol abuse, or myelodysplastic syndromes. High white blood cell count or blasts may be present in acute or chronic leukemia.
Step 2: Review peripheral smear. Make sure that it is not due to platelet clumping, also
known as spurious or psuedothrombocytopenia. Attention should be made to the
smear with regards to large platelets, schistocytes ![]() , hypersegmented as well as
hyposegmented neutrophils, blasts, etc.
, hypersegmented as well as
hyposegmented neutrophils, blasts, etc.
Step 3: History and physical examination can give clues as well. The following questions should be asked:
1. Previous history of thrombocytopenia or other blood related problems
2. Recent infections or illnesses
3. New medications
4. Previous blood transfusions
5. Risk factors for HIV
6. Alcohol abuse, etc.
7. Dietary habits Common tests in the diagnosis of thrombocytopenia are shown in Table 6 Anti-platelet or platelet associated antibodies are neither sensitive nor specific. The role of these tests is not well defined. If there is suspicion for TTP/ HUS (Hemolytic Uremic Symptom) ordering reticulocyte count, LDH and haptoglobin is highly recommended. HIV and hepatitis tests should be done only if the patient has risk factors.
Role of Bone Marrow Biopsy
Bone marrow aspiration/biopsy is minimally invasive, but usually is associated with pain/ pressure. This should be reserved for patients in whom the above work-up is unrevealing or if there is any suspicion for myelodysplastic syndrome or leukemia. It serves as a confirmatory test in immune thrombocytopenia (increased or adequate number of megakaryocytes), myelodysplastic syndrome (dysmegakaryopoiesis, etc.) or leukemia (increased number of blasts- >20%). Please refer to in Figure 1 and Figure 2.
Management
Treating the underlying cause is the most important intervention. If it is immune thrombocytopenic purpura, start appropriate treatment such as steroids or intravenous immunoglobulin (IVIG). If a drug is a suspect, discontinue the drug and observe. Drug-induced thrombocytopenia is usually immune mediated and is treated as immune thrombocytopenic purpura with steroids and IVIG. Heparin Induced thrombocytopenia (HIT) is potentially life threatening condition. If there is clinical suspicion all heparin must be discontinued and direct thrombin inhibitor (egg. Lepirudin) must be initiated. Plasma exchange must be initiated immediately if TTP is suspected. In HEELP syndrome, often delivery is indicated. HIV related thrombocytopenia often responds to Zidovidine.
Platelet transfusions are generally reserved for patients who are bleeding or have a platelet counts of <10,000/mcL. The main goal of transfusion is to prevent bleeding. If a patient is undergoing surgery or procedure, the target platelet count should be more than 75,000/mcL. Oprelvekin (Neumega) is an interleukin- 11, which has been shown to reduce the severity of thrombocytopenia due to chemotherapy and the need for platelet transfusions. It is not as widely used as other growth factors (filgastrim, erythropoietin) due to slow response, serious adverse reactions such as hypersensitivity reactions or anaphylaxis, significant fluid retention. The approach for outpatient and in-patient is quite different and is illustrated in Figure 1 and Figure 2.
References
1. Arepally GM, Ortel TL. Heparin-induced thrombocytopenia.. New England Journal of Medicine, 2006;355(8):809-17. [PubMed]
2. George JN, Vesely SK. Immune thrombocytopenic purpura--let the treatment fit the patient.. New England Journal of Medicine, 2003; 349:903. [PubMed]
3. Li X, Hunt L, Vesely SK. Drug-induced thrombocytopenia: an updated systematic review.Annals of Internal Medicine, 2005; 142:474. [PubMed]
4. Moake JL. Thrombotic microangiopathies. New England Journal of Medicine, 2002; 347:589-600. [PubMed]
5. Sekhon SS, Roy V. Thrombocytopenia in adults: A practical approach to evaluation and management. Southern Medical Journal, 2006;99(5):491-8. [PubMed]
6. Vanderschueren S, De Weerdt A, Malbrain M, et al. Thrombocytopenia and prognosis in intensive care. Critical Care Medicine. 2000;28(6):1871-6. [PubMed]
7. Von Drygalski A. Curtis BR, Bougie DW, et al. Vancomycin induced thrombocytopenia. New England Journal of Medicine, 2007; 356:904-910. [PubMed]
8. Warkentin TE, Aird WC and Rand JH. Platelet-Endothelial Interactions: Sepsis, HIT, and Antiphospholipid Syndrome. American Society of Hematology Education Program Book, 2003. [PubMed]
Table 1. Etiology of Thrombocytopenia
| Infectious | Non-infectious |
|---|---|
| Sepsis with or without disseminated intravascular coagulation | Medications |
| Hepatitis B and C | Nutritional deficiencies (B12, folate or iron deficiency) |
| HIV infection | Bone marrow problems |
| TTP/HUS | |
| HELLP syndrome | |
| Disseminated intravascular coagulation | |
| Alcohol | |
| Hypersplenism | |
| Post-transfusion purpura | |
| Acute pure megakaryocytic aplasia |
TTP/HUS = Thrombotic thrombocytopenic purpura/Hemolytic Uremic Symptom
HELLP – Hemolysis, elevated liver enzymes, low platelets
Table 2. Common medications causing thrombocytopenia
| Antimicrobials | Others |
|---|---|
| Piperacillin-tazobactam | Heparin |
| Trimethaprim-sulfamethoxazole | H2 blockers (e.g. Ranitidine) |
| Vancomycin | Quinine |
| Rifampin | Valproic acid |
| Ganciclovir | Glycoprotein IIb/IIIa inhibitors |
| Linezolid | Chemotherapy (e.g. Gemcitabine) |
Table 3. Congenital causes of thrombocytopenia
| Von-Willibrand disease type 2B |
| Wiskot-Aldrich syndrome |
| Alport syndrome |
| Fanconi’s anemia |
| Bernard-Soulier syndrome |
| Thrombocytopenia with absent radius syndrome |
Table 4. Etiology of thrombocytopenia in HIV patients.
| Primary HIV associated thrombocytopenia |
| Hypersplenism |
| Opportunistic infections |
| Malignancy (Lymphoma, etc.) |
| Medications |
| TTP/HUS* |
| Bone marrow problems (e.g. MDS) |
Table 5. Common clinical presentations of thrombocytopenia
| Petichial hemorrhages |
| Echymoses or bruising |
| Wet purpura, bleeding from mucus membranes of the mouth |
| Bleeding from nose, gums, hematuria, or heavy menstrual flow in females, etc. |
Table 6. Common tests in the evaluation of thrombocytopenia
| Complete blood count with differential |
| Reticulocyte count |
| LDH |
| Haptoglobin |
| B12, folate and iron levels |
| Anti-nuclear antibodies |
| HIV test |
| Hepatitis B and C antibodies |
| Platelet associated antibodies |
Figure 1. Algorithm for evaluation of thrombocytopenia as outpatient
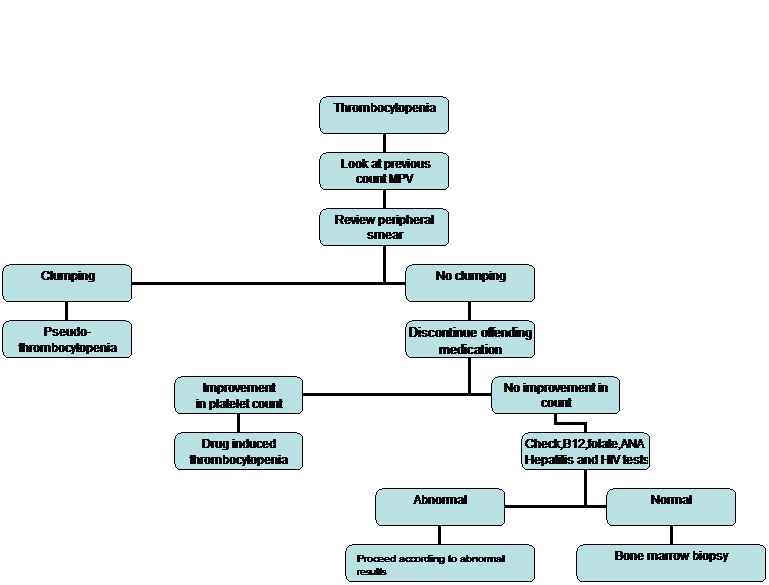
Figure 2. Algorithm for evaluation of thrombocytopenia for hospitalized patients

What's New
Yu XJ, et al. Fever with thrombocytopenia associated with a novel bunyavirus in China. N Engl J Med 2011;364:1523-1532.
GUIDED MEDLINE SEARCH FOR
Reviews
Ramaprasad C, Pursell K. Cytopenias after Solid Organ Transplantation.
GUIDED MEDLINE SEARCH FOR RECENT REVIEWS
History
Imbach P. Treatment of immune thrombocytopenia with intravenous immunoglobulin and insights for other diseases. A historical review. Swiss Medical Weekly 2012;142:w13593.
Blajchman MA. Platelet transfusions: an historical perspective. Hematology Am Soc Hematol Educ Program 2008;1:197.
Schwartz RS. Immune thrombocytopenia purpura--from agony to agonist. N Engl J Med 2007;357:2299-2301.
